Neuropathic Pain and Nociceptive Pain Topic
- Geriatric Use and Pediatric Use of Gabapentin for Neuropathic Pain
- Can a Vitamin B12 Deficiency Cause Sciatica?
- What is Neuropathic Pain and How to Live With Nerve Pain ?
- What Is The Difference Between Nociceptive and Neuropathic Pain ?
- The Causes of Nociceptive Pain, How is Nociceptive Pain Treated ?
- Gabapentin is Widely Used for Neuropathic Pain and Postherpetic Neuralgia
- What is Trigeminal Neuralgia ? Is Gabapentin a good Prescription for Trigeminal Neuralgia ?
- What is Gabapentin Used for ? What is the Off-Label Usages of Gabapentin ?
- Gabapentin for Chronic Neuropathic Pain and Fibromyalgia
- What is The Gate Control Theory ?
No Medication Pain Relief
- Why Is It Important to Find the Reasons of Pain ?
- Is Acetaminophen Safe ? Medicines Containing Acetaminophen
- Can Vitamin A Deficiency Lead to Pain ?
- The Deficiency in Certain Vitamins and Minerals Can Lead to Pains
- What is Joint Pain and How to Relieve Joint Pain Naturally?
- What Kinds of Nutrition and Nature Products Can Relieve Pain ?
- Why Biomedical Methods Can Be Used to Treat Migraine ?
- Table of Exempted Prescription Products 2023
- Is Acupuncture Effective for Migraines?
- Order Fioricet Pills with Free Prescription
- Herbal Natural Pain Killer Alternatives to Pain Relief Medicines
- How to Buy Medicines Safely From an Online Pharmacy
- How to Relieve your Pain Naturally ?
- Capsaicin Cream can Reduce Pain from Arthritis, Shingles, Neuropathy, Cluster Headache, and Skin Problems
- How to Treat Arthritis and Osteoarthritis
- What is The Gate Control Theory ?
- Relief from Arthritis Pain
- Neck Pain Reliever
- Tylenol Overdose Study
- Is Chronic Pain Medication Safe for Long- Term Use?
What is Nerve Pain ?
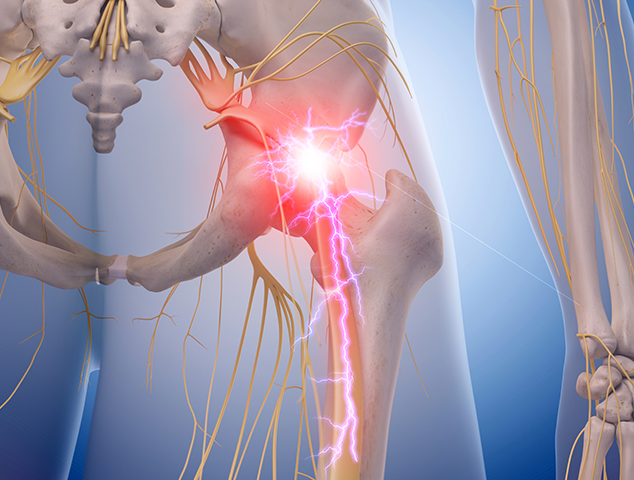
Nerve pain, also known as neuropathic pain, is a type of chronic pain that occurs due to damage or dysfunction in the nerves that transmit signals from various parts of the body to the brain and spinal cord. Unlike nociceptive pain, which results from physical injury to tissues (such as a cut or a bruise), neuropathic pain arises from abnormalities within the nervous system itself. Here’s a detailed explanation:
Characteristics of Nerve Pain
- Sensation Quality:
- Burning or Scalding: A persistent, painful burning sensation.
- Tingling or “Pins and Needles”: A prickling or tingling feeling, often described as “pins and needles.”
- Electric Shock: Sudden, sharp, and shooting pain that feels like an electric shock.
- Stabbing or Piercing: Intense, sharp, and stabbing pain.
- Numbness: A loss of sensation in the affected area.
- Duration:
- Can be constant or intermittent.
- Often chronic, persisting for months or even years.
- Distribution:
- Can affect a specific nerve (localized) or multiple nerves (generalized).
- Commonly occurs in extremities like hands and feet but can occur anywhere in the body.
- Sensitivity:
- Allodynia: Pain from stimuli that don’t usually cause pain (e.g., a light touch or mild temperature change).
- Hyperalgesia: Increased sensitivity to painful stimuli.
Causes of Nerve Pain
- Diabetes: High blood sugar levels can damage nerves over time (diabetic neuropathy).
- Injuries: Physical trauma, such as from an accident or surgery, can damage nerves.
- Infections: Certain infections, like shingles (herpes zoster), can affect nerves.
- Autoimmune Diseases: Conditions like multiple sclerosis or lupus where the immune system attacks the nervous system.
- Nutritional Deficiencies: Lack of essential vitamins, particularly B vitamins, can lead to nerve damage.
- Toxins: Exposure to certain chemicals or toxins, including chemotherapy drugs, can cause neuropathy.
- Genetic Disorders: Some inherited conditions, like Charcot-Marie-Tooth disease, affect the nerves.
- Tumors: Both benign and malignant tumors can press on nerves.
- Idiopathic: Sometimes, the cause of nerve pain is unknown.
Diagnosis of Nerve Pain
Diagnosing neuropathic pain involves a thorough medical history, physical examination, and various diagnostic tests, such as:
- Neurological Examination: To assess sensation, reflexes, and muscle strength.
- Electromyography (EMG) and Nerve Conduction Studies: To evaluate the electrical activity of muscles and the speed of nerve signals.
- Imaging Tests: MRI or CT scans to detect structural problems.
- Blood Tests: To identify underlying conditions like diabetes or nutritional deficiencies.
- Nerve Biopsy: In rare cases, a small sample of nerve tissue is taken for examination.
Impact of Nerve Pain
Nerve pain can significantly affect quality of life, leading to physical limitations, emotional distress, and sleep disturbances. It often requires a comprehensive and multidisciplinary approach for effective management, including medications, physical therapy, psychological support, and sometimes surgical interventions.
How Are Nerve Pain and Nerve Damage Treated?
Nerve pain (neuropathic pain) and nerve damage are treated through a combination of medications, therapies, and sometimes surgical interventions. The treatment approach often depends on the underlying cause, severity, and individual patient factors. Here’s an overview of the common treatments:
Medications
- Pain Relievers:
- Over-the-counter options like ibuprofen or acetaminophen.
- Prescription pain medications, including opioids, may be used for severe pain but are generally avoided due to the risk of addiction and side effects.
- Antidepressants:
- Tricyclic antidepressants (e.g., amitriptyline, nortriptyline) are often effective for neuropathic pain.
- Serotonin-norepinephrine reuptake inhibitors (SNRIs) like duloxetine and venlafaxine.
- Anticonvulsants:
- Medications like gabapentin and pregabalin are commonly prescribed for nerve pain.
- Topical Treatments:
- Creams, gels, or patches containing lidocaine or capsaicin can provide localized relief.
- Steroids:
- Corticosteroids may be used to reduce inflammation that is causing nerve compression or irritation.
Non-Medication Therapies
- Physical Therapy:
- Helps improve strength, flexibility, and function.
- Techniques such as TENS (transcutaneous electrical nerve stimulation) can provide pain relief.
- Occupational Therapy:
- Assists patients in managing daily activities and adapting to any physical limitations.
- Cognitive Behavioral Therapy (CBT):
- Helps patients manage chronic pain by changing the way they think and react to pain.
- Acupuncture:
- May provide relief for some individuals through the insertion of thin needles at specific points on the body.
- Biofeedback:
- Uses electronic monitoring to teach patients how to control certain body functions that can alleviate pain.
Surgical and Other Interventions
- Nerve Blocks:
- Injections of anesthetics, steroids, or other medications near nerves can reduce pain.
- Surgery:
- May be necessary to relieve pressure on a nerve (e.g., carpal tunnel syndrome) or to repair damaged nerves.
- Implantable Devices:
- Spinal cord stimulators or peripheral nerve stimulators can help control chronic pain by sending electrical impulses to the nerves.
Lifestyle and Home Remedies
- Exercise:
- Regular physical activity can improve overall health and reduce nerve pain symptoms.
- Healthy Diet:
- Proper nutrition supports nerve health and overall well-being.
- Good Sleep Hygiene:
- Adequate and restful sleep is crucial for managing pain.
- Stress Management:
- Techniques like meditation, yoga, or deep-breathing exercises can help reduce pain perception.
Treatment of Underlying Conditions
If nerve pain or damage is due to an underlying condition (e.g., diabetes, shingles, autoimmune diseases), treating that condition is essential. This may involve managing blood sugar levels, antiviral medications, or immunosuppressive drugs.
Multidisciplinary Approach
Often, a combination of treatments is necessary for optimal pain management. A multidisciplinary approach involving healthcare providers from various specialties (neurology, pain management, physical therapy, psychology) can be beneficial.
Follow-up and Monitoring
Regular follow-up with healthcare providers is important to monitor the effectiveness of treatments, adjust therapies as needed, and manage any side effects.