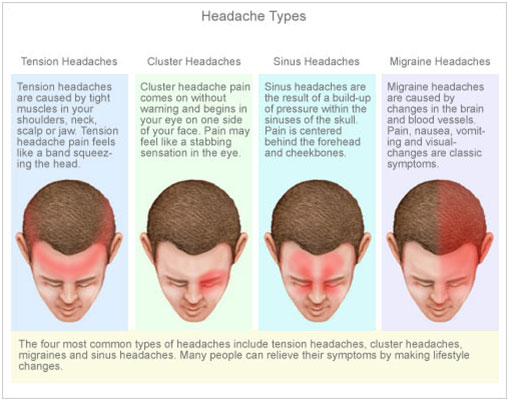
A tension headache is the most common type of headache. It is pain or discomfort in the head, scalp, or neck, and is often associated with muscle tightness in these areas.
Tension-type headache is a neurological disorder characterised by a predisposition to attacks of mild to moderate headache with few associated symptoms.
The diagnosis is based on the history and examination. Over the past few decades research on headache has centred on migraine, and much of the best quality evidence for the treatment of tension-type headache is decades old. Some consensus based treatment guidelines are available (see Additional Educational Resources box towards the end of this article).
Treatment has changed little over the past two decades. Many patients self treat acute attacks and seek advice when attacks become frequent or chronic. This review focuses on how to identify and manage patients who require medical advice about acute attacks and preventive treatment to minimise further attacks.
Diagnostic criteria for tension-type headache
(A) At least 10 episodes fulfilling the criteria B-D:
(B) Headache lasting from 30 minutes to 7 days
(C) Headache has at least two of the following characteristics:
Bilateral location
Pressing/tightening (non-pulsating) quality
Mild or moderate intensity
Not aggravated by routine physical activity such as walking or climbing stairs
(D) Both of the following:
No nausea or vomiting (anorexia may occur)
No more than one episode of photophobia or phonophobia
(E) Not attributable to another disorder
Infrequent episodic tension-type headache
Diagnosed if headaches meeting the above criteria occur <1 day a month (<12 days a year) on average
Frequent episodic tension-type headache
Diagnosed if headaches occur >1 and <15 days a month (>12 and <180 days a year).
Chronic tension-type headache
Diagnosed if headaches occur ≥15 days a month (180 or more days a year).
*Adapted from the second revision of the international classification of headache disorders
Causes of Tension Headache
Tension headaches occur when neck and scalp muscles become tense or contract. The muscle contractions can be a response to stress, depression, head injury, or anxiety.
They may occur at any age, but are most common in adults and older teens. It is slightly more common in women and tends to run in families.
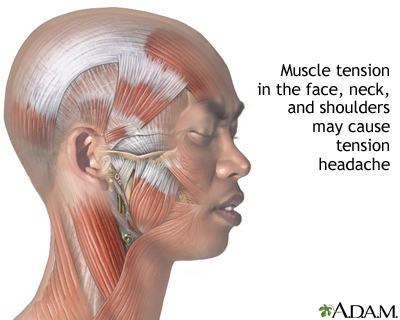 Any activity that causes the head to be held in one position for a long time without moving can cause a headache. Activities may include typing or other computer work, fine work with the hands, and using a microscope. Sleeping in a cold room or sleeping with the neck in an abnormal position may also trigger a tension headache.
Any activity that causes the head to be held in one position for a long time without moving can cause a headache. Activities may include typing or other computer work, fine work with the hands, and using a microscope. Sleeping in a cold room or sleeping with the neck in an abnormal position may also trigger a tension headache.
Other triggers of tension headaches include:
- Physical or emotional stress
- Alcohol use
- Caffeine (too much or withdrawal)
- Colds, the flu, or a sinus infection
- Dental problems such as jaw clenching or teeth grinding
- Eye strain
- Excessive smoking
- Fatigue or overexertion
Tension headaches can occur when you also have a migraine. Tension headaches are not associated with brain diseases.
How should tension-type headache be treated?
Treatment for tension-type headache includes acute therapy for individual attacks and preventive treatment to minimize the number of attacks that occur. Acute and preventive treatment can be used together.
Individual headache attacks
Acute attacks of tension-type headache are usually treated with simple analgesics. Oral aspirin 500-1000 mg has the best evidence of effectiveness in randomized controlled trials. In one study, 75% of participants reported relief of headache two hours after aspirin and success was not affected by pain intensity at the time of treatment. Other non-steroidal anti-inflammatory drugs also are effective, suggesting a class effect. Gastric irritation and occasionally ulceration may complicate treatment with aspirin or other non-steroidal anti-inflammatory drugs, even when they are used intermittently. Evidence for paracetamol (acetaminophen) from randomized controlled trials is mixed. It is probably more effective than placebo, but inferior to non-steroidal anti-inflammatory drugs.
Randomized controlled trials show that combination drugs containing simple analgesics and caffeine are also effective for acute treatment of tension-type headache. Many drugs used for acute treatment of tension-type headache are available to patients without a prescription, making it difficult for the doctor to monitor use.
Opioids or sedative hypnotics should not be used routinely to treat tension-type headache because they impair alertness and are common causes of overuse and dependence syndromes. Evidence from case-control and cohort studies shows that opioids increase the risk of chronic headache. Once established, all forms of medication overuse are difficult to treat, and recidivism is common. Clinical vigilance to prevent medication overuse is among the most important responsibilities of the doctor caring for a patient with headache.
Preventive Treatment of Tension Headache
Daily preventive treatment should be considered for patients with frequent headaches or who respond poorly to abortive treatment (pain reducing treatment) alone. The risk of developing more frequent headaches over time is confined principally to patients with at least two headaches a month, and the risk increases exponentially once headaches are weekly, suggesting that preventive treatment should be considered at or before this point.
Clinical experience and evidence from case series and cohort studies suggest that the benefit of preventive treatment is diminished when patients are simultaneously overusing abortive treatments. In most cases, withdrawal of medication is advisable before starting preventive treatment.
The best evidence of effectiveness from randomized controlled trials is for amitriptyline, usually in doses of 75-150 mg a day. In addition to its effects on pain, amitriptyline decreases muscle tenderness. Its effect is augmented by the addition of relaxation or tizanidine. Amitriptyline also is effective for migraine prophylaxis, making it a good choice for patients who have both forms of headache. Common side effects of amitriptyline include dry mouth, sedation, constipation, and blurred vision. Weight gain is the most common side effect that limits treatment, occurring in up to a quarter of patients.
The headache benefits of amitriptyline are unlikely to stem from its antidepressant actions as the effective dose is generally lower than the dose needed to treat depression. Additionally, other drugs effective against depression, such as selective serotonin reuptake inhibitors, are not effective for tension-type headache.
Compared with amitriptyline, other preventive treatments for tension-type headache have far less rigorous evidence of benefit. There is modest evidence from randomized controlled trials that tizanidine, an α agonist, is helpful for chronic tension-type headache in doses up to 18 mg a day. Side effects include sedation and dry mouth. One trial showed benefit for mirtazapine 15-30 mg a day. Randomized controlled trials consistently show no benefit for botulinum toxin type A injections into the pericrania muscles.
Clinical experience suggests that side effects are minimized and compliance increased when preventive treatment is started at a low dose and gradually increased until the target dose is reached. A common practice is to increase the dose at weekly intervals. Headaches naturally wax and wane, so two or three months of preventive treatment at the target dose is recommended before outcomes can be judged. A headache diary provides objective confirmation of treatment effects.
The usual goals of treatment are a reduction in the frequency and intensity of headache and improved response to abortive treatment. The optimal duration of preventive treatment is unknown. In the absence of evidence, a reasonable practice is to continue a successful preventive regimen for six months and then slowly reduce the dose while observing headache frequency. Treatment can be resumed if headaches recur.
The List the Medications for Tension Headache
Tension headaches are among the most common types of headaches, often characterized by a dull, aching pain and tightness or pressure around the forehead or back of the head and neck. They are typically treated with a combination of over-the-counter (OTC) medications, prescription medications, and sometimes non-drug therapies. Below is a detailed list of medications used for treating tension headaches:
1. Over-the-Counter (OTC) Medications
These medications are commonly available without a prescription and are typically used for mild to moderate tension headaches.
a. Nonsteroidal Anti-Inflammatory Drugs (NSAIDs):
- Ibuprofen (Advil, Motrin): Reduces inflammation and pain. Typical dose: 200-400 mg every 4-6 hours, with a maximum of 1200 mg/day for OTC use.
- Naproxen (Aleve): Longer-acting NSAID for pain relief. Typical dose: 220 mg every 8-12 hours, with a maximum of 660 mg/day for OTC use.
- Aspirin (Bayer, Bufferin): Relieves pain and inflammation. Typical dose: 325-650 mg every 4-6 hours, with a maximum of 4000 mg/day.
b. Acetaminophen (Tylenol):
- Commonly used for pain relief. It does not reduce inflammation like NSAIDs but is gentler on the stomach. Typical dose: 325-650 mg every 4-6 hours, with a maximum of 3000 mg/day.
c. Combination Medications:
These combine multiple active ingredients for enhanced pain relief.
- Excedrin Tension Headache: Contains acetaminophen and caffeine. The caffeine enhances the pain-relieving effects of acetaminophen. Typical dose: 2 caplets every 6 hours, with a maximum of 6 caplets per day.
2. Prescription Medications
For chronic or severe tension headaches, prescription medications may be required.
a. Prescription NSAIDs:
- Diclofenac (Voltaren): Available in both oral and topical forms. Typically prescribed in doses of 50-75 mg two or three times a day.
- Indomethacin: Stronger NSAID used for severe headaches. Typical dose: 25-50 mg two or three times daily.
b. Muscle Relaxants:
These are sometimes prescribed when tension headaches are linked to muscle tightness in the neck and shoulders.
- Cyclobenzaprine (Flexeril): Used to reduce muscle tension and pain. Typical dose: 5-10 mg, three times a day.
- Tizanidine (Zanaflex): Relieves muscle spasms and tightness. Typical dose: 2-4 mg, three times a day.
c. Tricyclic Antidepressants (TCAs):
Used for chronic tension-type headaches as a preventive treatment.
- Amitriptyline: Most commonly prescribed TCA for tension headaches. Typical dose: 10-25 mg at bedtime.
- Nortriptyline (Pamelor): A similar option, typically prescribed in doses of 10-75 mg/day.
d. Selective Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs):
SNRIs can help manage chronic tension headaches by affecting serotonin and norepinephrine levels.
- Venlafaxine (Effexor): Used in some cases to prevent headaches. Typical dose: 75-150 mg/day.
3. Preventive Medications
For individuals with chronic tension headaches, preventive medications might be used on a daily basis to reduce the frequency and severity of headaches.
a. Beta-Blockers:
- Propranolol: Primarily used for migraine prevention but may be prescribed for tension headaches as well. Typical dose: 40-160 mg/day.
b. Anticonvulsants:
- Gabapentin (Neurontin): May be used to prevent chronic tension headaches by reducing nerve pain. Typical dose: 300-1800 mg/day, depending on response.
c. Botulinum Toxin (Botox):
- In some cases, Botox injections may be used to prevent chronic tension headaches by relaxing muscles in the head and neck area.
4. Caffeine-Containing Medications
- Fioricet: A prescription combination of acetaminophen, caffeine, and butalbital (a barbiturate). Butalbital is a sedative that relaxes muscles and relieves tension. Typical dose: 1-2 tablets every 4 hours, with a maximum of 6 tablets per day.
- Fiorinal: Similar to Fioricet but contains aspirin instead of acetaminophen. It also contains caffeine and butalbital. Typical dose: 1-2 tablets every 4 hours, with a maximum of 6 tablets per day.
5. Non-Pharmacological Approaches
While these are not medications, they are often recommended alongside medical treatment for tension headaches.
- Biofeedback: Helps patients control muscle tension.
- Physical Therapy: Targets neck and shoulder muscles to reduce tension.
- Cognitive Behavioral Therapy (CBT): Helps manage stress, which may trigger headaches.
- Acupuncture: May provide relief in some cases.
Important Considerations:
- Overuse of pain relievers, particularly OTC medications like NSAIDs and acetaminophen, can lead to medication-overuse headaches (rebound headaches).
- Chronic tension headaches should be managed under a healthcare provider’s supervision, as long-term use of some medications (e.g., muscle relaxants, antidepressants) may have side effects.
The Treatment of Tension Headache
Is Fioricet a Good Prescription for Tension Headache ?