Whether it’s due to stress, lack of sleep, or the result of a few glasses of wine, there are many reasons you may experience a……
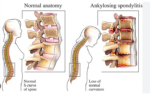
The treatment of Ankylosing Spondylitis (AS) focuses on reducing inflammation, relieving pain, and slowing the progression of the disease. Below is a detailed list of……
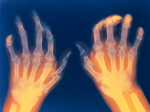
What is Inflammatory Arthritis ? Inflammatory arthritis is a term used to describe a group of chronic, autoimmune disorders characterized by inflammation in the joints.……
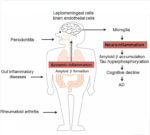
Internal inflammation, also known as systemic inflammation, can manifest in various ways, and its symptoms can vary depending on the underlying cause and severity of……
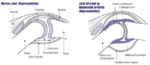
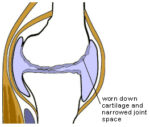
What is Joint Pain ? Joint pain refers to discomfort, soreness, or aching sensations in one or more of the body’s joints. Joints are the……
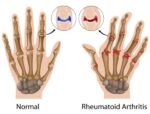
Many people think that there is no cure to unbearable arthritis pain especially in case of osteoarthritis, but many people suffering from rheumatoid arthritis believe……
An active component of chile pepper, capsaicin temporarily desensitizes pain-prone skin nerve receptors called C-fibers; soreness is diminished for 3 to 5 weeks while they……
Although there is no miracle cure for arthritis, does not mean that there are ways to relieve pain and discomfort caused by arthritis. One way……
The name arthritis refers to a not only one disease, but to a whole grouping of over 100 different forms of a disease. It is……
About 1 in 4 adults in the United States have arthritis, a leading cause of disability. Healthy People 2030 focuses on reducing pain, disability, and limitations……
Sudden, painful swelling at the base of the big toe is often the first warning sign of gout. It can affect other joints as well.……