Back pain is a common condition that can be caused by a variety of factors, including muscle strain, disc degeneration, arthritis, and nerve compression. The……
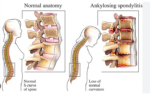
The treatment of Ankylosing Spondylitis (AS) focuses on reducing inflammation, relieving pain, and slowing the progression of the disease. Below is a detailed list of……
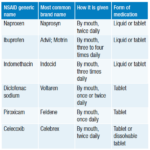
Nonsteroidal anti-inflammatory drugs (NSAIDs) are widely used to treat a variety of pain and inflammation conditions. They are effective because they block the production of……
The largest group of over-the-counter painkillers are the non-steroidal anti-inflammatory drugs (NSAIDs). As their name suggests, they also reduce inflammation but – unlike other anti-inflammatory……
Gabapentin is an anti-seizure and nerve pain medication. its dosage range for various conditions, and some of its potential side effects. To recap: Off-Label Uses:……
Non-steroidal anti-inflammatory drugs (NSAIDs) are medicines that are widely used to relieve pain, reduce inflammation, and bring down a high temperature. They’re often used to……
Paracetamol (acetaminophen) is generally considered to be a weak inhibitor of the synthesis of prostaglandins (PGs). However, the in vivo effects of paracetamol are similar……
The following possible side effects of medicines for gout are listed by the U.S. Food and Drug Administration (FDA) and in reports from research. Just……
Treatment of chronic pain usually involves medicines and therapy. Medicines used for chronic pain include pain relievers, antidepressants and anticonvulsants. Different types of medicines help……
In some cases wherein people suffer from severe back pain, pain medication becomes quite necessary to treat the pain. Pain medication can be given to……
When your pet hound matures, it will require a more specialized and focused attention and care in the same way that we provide old people.……
Ask a typical shopper if you could reduce inflammation without NSAIDS and see what response you will get. My guess is they would ask what……
What is Acetaminophen? Acetaminophen is a pain reliever and a fever reducer. Acetaminophen is used to treat many conditions such as headache, muscle aches, arthritis,……