Trigeminal Neuralgia is a sever neuropathic disorder of the facial nerve. It is characterized by serious bouts of pain in the facial region. This pain generally originates from the Trigeminal nerve in the face. Patients affected by this disease generally feel the pain in the eyes, ear, nose, forehead , cheeks, jaw and side of the face. In some cases the pain may be felt in the left index finger also.
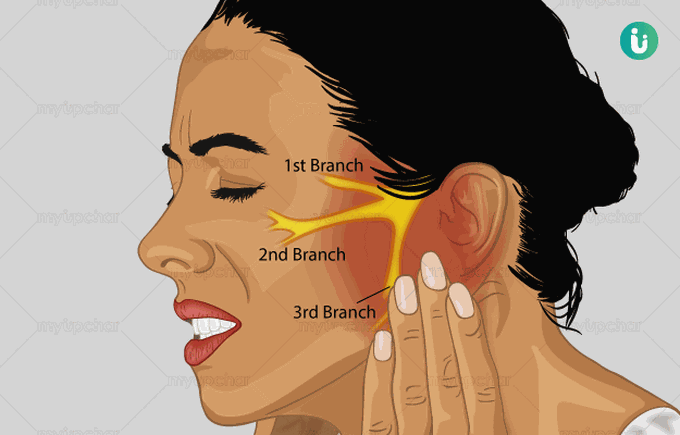
The duration of the attack may last from a few seconds to several minutes or hours. Researches reveal that people above 50 years get affected and the percentage is more in females than in males.
Trigeminal neuralgia refers to lancinating pain in the 2nd and 3rd divisions of the trigeminal nerve, which is the 5th cranial nerve. It usually occurs in patients over 50 years of age.
The exact mechanism of the disease is not known. It is thought to be caused by vascular compression i.e. an aberrant loop of the cerebellar arteries compressing the trigeminal nerve as it enters the brain.
Patients usually present with a severe, repetitive, knife-like pain on the face. The pain can be triggered by touching the face, eating, cold wind blowing on the face, and by pronouncing certain words.
What is trigeminal neuralgia?
Trigeminal neuralgia is a condition characterized by pain coming from the trigeminal nerve, which starts near the top of the ear and splits in three, toward the eye, cheek and jaw. We have two trigeminal nerves for each side of our face, but trigeminal neuralgia pain most commonly affects only one side.
The pain of trigeminal neuralgia is unlike facial pain caused by other problems. It is often described as stabbing, lancinating or electrical in sensation and so severe that the affected person cannot eat or drink. The pain travels through the face in a matter of seconds, but as the condition progresses, the pain can last minutes and even longer.
Trigeminal neuralgia is sometimes known as tic douloureux, which means “painful tic.”
Causes of Trigeminal Neuralgia
Trigeminal neuralgia usually occurs spontaneously, but is sometimes associated with facial trauma or dental procedures.
The condition may be caused by a blood vessel pressing against the trigeminal nerve, also known as vascular compression. Over time, the pulse of an artery rubbing against the nerve can wear away the insulation, which is called myelin, leaving the nerve exposed and highly sensitive.
The resulting symptoms can be similar to those caused by dental problems, and sometimes people with undiagnosed trigeminal neuralgia explore multiple dental procedures in an effort to control the pain.
Multiple sclerosis or a tumor — while rare — can also cause trigeminal neuralgia. Researchers are exploring whether or not postherpetic neuralgia (caused by shingles) can be related to this condition.
Trigeminal Neuralgia Symptoms
Trigeminal neuralgia occurs more often in women than men, is more common in older people (usually 50 and older), and occurs more on the right than the left. It doesn’t usually run in families.
Trigeminal neuralgia symptoms may include:
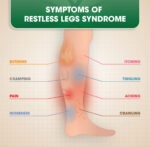
- Episodes of sharp, intense, stabbing pain in the cheek or jaw that may feel like an electric shock. Pain episodes may be triggered by anything touching the face or teeth, including shaving, applying makeup, brushing teeth, touching a tooth or a lip with the tongue, eating, drinking or talking — or even a light breeze or water hitting the face.
- Periods of relief between episodes.
- Anxiety from the thought of the pain returning.
What are typical symptoms?
Very painful, sharp, electric-like jolts of pain that last a few seconds or minutes. Pain is only on one side of the face, usually around the eye, cheek, lips, and lower part of the face. Pain may be triggered by:
- Brushing your teeth or hair
- Chewing, drinking, or eating
- Shaving, washing, or wind
Trigeminal Neuralgia Pain
The trigeminal nerve splits off into three branches: ophthalmic, maxillary and mandibular. Each branch provides sensation to different areas of the face. Depending on which branch and which part of the nerve is irritated, trigeminal neuralgia pain can be felt anywhere in the face. Most commonly, it is felt in the lower part of the face. The intensity of the pain is exceptional: Some people report it to be more severe than experiencing a heart attack, passing a kidney stone or even giving birth.
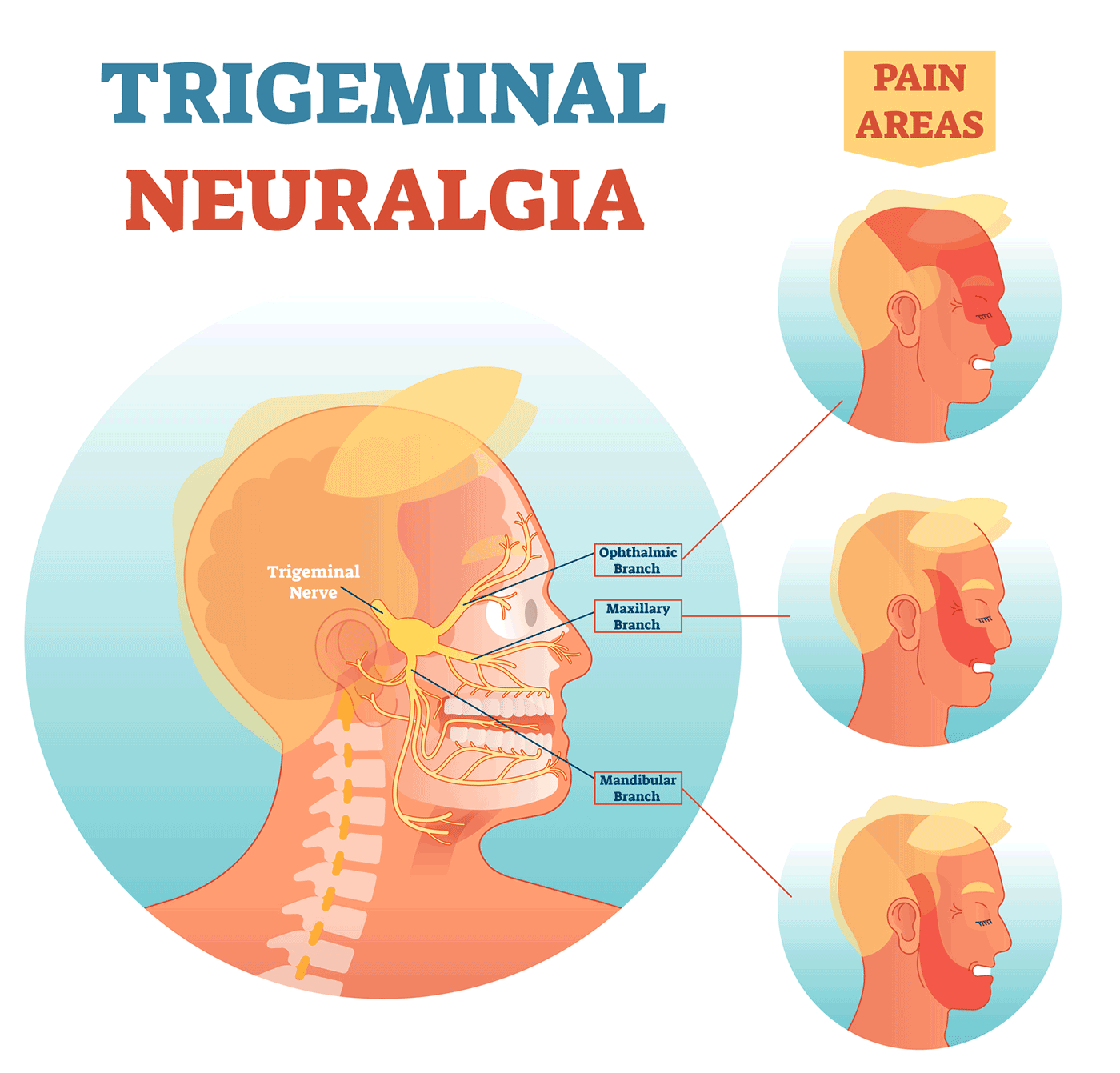
A flare-up of trigeminal neuralgia may begin with tingling or numbness in the face. Pain occurs in intermittent bursts that last anywhere from a few seconds to two minutes, becoming more and more frequent until the pain is almost continuous.
Flare-ups may continue for a few weeks or months followed by a pain-free period that can last a year or more. Although trigeminal neuralgia pain may seem to disappear, it always comes back, often with more intensity.
In some cases, instead of sharp, stabbing pain, trigeminal neuralgia appears as a persisting dull ache. This and other symptom variations are sometimes described as “atypical trigeminal neuralgia.”
Trigeminal Neuralgia Diagnosis
Diagnosing trigeminal neuralgia involves a physical exam and a detailed medical history to rule out other causes of facial pain. Your health care provider (usually your primary care doctor or a neurologist) will ask about the frequency and intensity of the pain, what seems to set it off and what makes it feel better or worse. Since there is no single test for trigeminal neuralgia, getting to the nature of the pain is key to the diagnosis.
Your provider may also recommend imaging or laboratory tests, such as a CAT scan or a high-resolution MRI of the trigeminal nerve and surrounding areas. These tests can help determine if the pain is caused by a tumor or blood vessel abnormality, or by undiagnosed multiple sclerosis. Certain advanced MRI techniques may help the doctor see where a blood vessel is pressing against a branch of the trigeminal nerve.
There has been much debate about the causes of Trigeminal Neuralgia. According to new age researches the cause is an ‘enlarged blood vessel’ which in turn compresses or rubs the Trigeminal nerve in the region where it meets the pons. Such severe compression causes episodes of pain.
Unfortunately in many cases Trigeminal Neuralgia has been wrongly diagnosed as some dental problem.
However, to manage the pain and cure the disease it needs early treatment. Surgery is recommended many a times to cure the disease. It is done either to relieve the compression or to damage it in a way so that the brain stops receiving the pain signals during episodes of attack. Surgery, if done with expert hands has a success rate of 90 per cent.
Diagnosis is mainly clinical. Carbamazepine is mostly prescribed to the patients for treatment. Surgical options include injection of alcohol or phenol into the peripheral branch of the nerve and surgical decompression of the nerve through a posterior craniotomy approach.
Trigeminal Neuralgia Treatment
Most common over-the-counter and prescription pain medicines don’t work for people with trigeminal neuralgia, but many modern treatments can reduce or eliminate the pain. The doctor may recommend one or more of these approaches:
Trigeminal Neuralgia Medications
Many people who suffer from trigeminal neuralgia successfully manage this condition for many years with medication. Trigeminal neuralgia drug therapy uses some of the same medicines prescribed for controlling seizures, which includes carbamazepine, gabapentin and similar agents. Regular blood tests may be required for some medications to check your white blood cell count, platelets, sodium levels and liver function.
Your neurologist or primary care physician can help you select the best drug and the most appropriate dosage. Most patients start out on low doses, gradually increasing the dose under clinical supervision until they achieve the best pain relief with the least amount of side effects.
Antivasculants are usually prescribed by the doctors as medication for Trigeminal Neuralgia. Carbamazepine if the first choice and is used as the first line of drug. Others include phenytoin, gabapentin, lamotrigine, baclofen, and oxcarbazepine.
Young patients suffering from Trigeminal Neuralgia syndrome may sometimes sink into depression. It is therefore very important to reassure them that treatment for this chronic pain disease exists.
Trigeminal Nerve Blocks
Nerve blocks are injections (with a steroid medication or another agent) made at various parts of the nerve to reduce pain. They may provide temporary pain relief for people with trigeminal neuralgia. Multiple injections are usually needed to achieve the desired relief, and the effects may have different durations for different people.
Patients who have been suffering from Trigeminal Neuralgia identify a specific ‘trigger area’ in their face. This area is so sensitive that mere touching or even air currents may initiate the attacks. Common activities like eating, talking and even brushing the teeth can initiate a severe attack. Patients have described the pain to be stabbing, shocking, burning, pressing, crushing, exploding and even shooting. In extreme cases, one, two or all three branches of the trigeminal nerve may be affected.
Stereotactic radiation therapy is also used as a treatment for this problem. No surgery or incisions are used in this procedure. It uses targeted radiation to bombard the nerve. However, this treatment is generally recommended for patients who are not fit for surgery.
Surgery for Trigeminal Neuralgia
If medication no longer controls your trigeminal neuralgia pain despite the increased dosage, or if the side effects are intolerable, there are several surgical procedures to consider. It helps to learn about these options before you are in urgent need of relief so you and your doctor have time to evaluate them. Your overall health, age, pain level and the availability of the procedure will all factor in to this decision. Most people with trigeminal neuralgia are candidates for any of the surgical treatment options — your doctor can help you decide which ones and in what order you should consider them.
The surgery for trigeminal neuralgia is delicate and precise since the involved area is very small. Look for experienced neurosurgeons who see and treat a large number of people with trigeminal neuralgia.
Rhizotomy
There are several kinds of rhizotomies for trigeminal neuralgia, which are all outpatient procedures performed under general anesthesia in the operating room. The surgeon inserts a long needle through the cheek on the affected side of the face and uses an electrical current (heat) or a chemical (glycerin or glycerol) to deaden the pain fibers of the trigeminal nerve. For those undergoing trigeminal neuralgia rhizotomy for the first time, the chemical approach is typically recommended. Those who have the procedure repeated often benefit from both the chemical and the heat treatment delivered in the same session.
The procedure takes about 30 minutes and most patients go home several hours later with less to no pain. Out of the three surgical options, rhizotomy offers the most immediate relief from trigeminal neuralgia pain. You may experience some swelling or bruising of the cheek. Your doctor will prescribe pain medications and, if necessary, give you a plan to gradually discontinue your medications.
Rhizotomy provides pain relief to about 80% of patients with trigeminal neuralgia, but it’s a temporary solution that usually lasts one to three years, until the nerve regrows.
Rhizotomy is a recommended surgical treatment for patients with trigeminal neuralgia resulting from multiple sclerosis (MS). It is minimally invasive and can be safely repeated, since the pain is more likely to come back due to the progression of MS.
Pain Medications, Pain Relief, and Pain Management