A migraine is a type of recurrent headache disorder characterized by moderate to severe throbbing or pulsating head pain, often on one side of the head. Migraines are typically accompanied by other symptoms, which can include nausea, vomiting, sensitivity to light (photophobia), and sensitivity to sound (phonophobia). These symptoms can significantly disrupt a person’s daily activities and quality of life.

Key features and characteristics of migraines include:
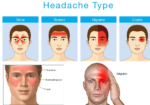
- Pain Characteristics: Migraine pain is often described as pulsating or throbbing and is usually located on one side of the head, although it can affect both sides in some cases. The pain is often severe and can last for hours to days.
- Aura (in Some Cases): Some people with migraines experience a visual or sensory disturbance known as an aura before the headache begins. Auras can include flashing lights, zigzag lines, blind spots, or tingling sensations in the face or hands. Not all migraine sufferers experience auras.
- Duration: Migraines can last anywhere from a few hours to several days. They are typically divided into two main phases: the prodrome phase (warning signs that can occur hours or days before the headache) and the attack phase (the actual headache episode).
- Triggers: Migraines can be triggered or exacerbated by various factors, including stress, hormonal changes (such as menstruation or menopause), certain foods or beverages, changes in sleep patterns, bright lights, loud noises, strong odors, and weather changes.
- Nausea and Vomiting: Many individuals with migraines experience nausea and vomiting during an attack, which can further intensify the discomfort.
- Sensory Sensitivity: Migraine attacks often make individuals highly sensitive to light and sound. They may seek out dark, quiet environments during an episode.
- Physical Activity Worsens Symptoms: Routine physical activities, such as climbing stairs, can exacerbate migraine symptoms.
- Postdrome Phase: After the headache subsides, some individuals experience a postdrome phase characterized by fatigue, mood changes, and difficulty concentrating.
- Family History: Migraines often run in families, suggesting a genetic component to the disorder.
Migraines are a complex neurological condition, and their exact cause is not fully understood. They are thought to involve a combination of genetic, environmental, and neurochemical factors. Changes in the brain’s blood flow, along with the release of various chemicals, including serotonin and calcitonin gene-related peptide (CGRP), are believed to play a role in migraine development.
Why Biomedical Methods Can Be Used to Treat Migraine ?
Biomedical methods can be used to treat migraines because they aim to target the underlying physiological and biochemical processes that contribute to migraine attacks. These methods often involve medications and therapeutic approaches designed to prevent or alleviate migraine symptoms. Here are some key reasons why biomedical methods are effective for treating migraines:
- Targeting Neurochemical Imbalances: Migraines are believed to involve changes in the brain’s neurochemical balance, including alterations in serotonin levels. Medications like triptans, serotonin receptor agonists, and serotonin-norepinephrine reuptake inhibitors (SNRIs) can help restore normal neurochemical function and alleviate migraine symptoms.
- Vasoconstriction: Some migraines are associated with the dilation of blood vessels in the brain. Medications like ergotamines and triptans work by constricting these blood vessels, reducing blood flow and relieving the associated pain.
- Preventative Therapy: Biomedical methods also include preventative or prophylactic treatments aimed at reducing the frequency and severity of migraine attacks. These may include beta-blockers, calcium channel blockers, anticonvulsants, and monoclonal antibodies like CGRP inhibitors.
- Pain Relief: Over-the-counter and prescription pain relievers, such as nonsteroidal anti-inflammatory drugs (NSAIDs), acetaminophen, and opioid medications, can provide relief from migraine pain when taken as directed.
- Nausea and Vomiting Control: Many migraine sufferers experience nausea and vomiting during attacks. Biomedical methods include medications like antiemetics (e.g., metoclopramide) to control these symptoms.
- Inflammatory Response: Migraine attacks can trigger an inflammatory response in the body. Nonsteroidal anti-inflammatory drugs (NSAIDs) and corticosteroids can help reduce inflammation and provide relief.
- Stress and Muscle Tension: Biomedical methods also consider the role of stress and muscle tension in migraine development. Muscle relaxants and medications for anxiety and depression may be prescribed to address these factors.
- Hormonal Influences: Hormonal fluctuations can trigger migraines in some individuals, especially in the case of menstrual migraines. Hormone therapy, including birth control pills and hormone replacement therapy (HRT), may be used to stabilize hormonal levels and reduce the frequency of attacks.
- Treatment Personalization: Biomedical approaches allow for individualized treatment plans based on the specific characteristics of a patient’s migraines. Healthcare providers can tailor medication choices and dosages to optimize effectiveness and minimize side effects.
- Clinical Trials and Research: Biomedical methods benefit from ongoing research and clinical trials that explore new medications, therapeutic approaches, and potential migraine targets. This continuous research contributes to the development of more effective treatments over time.
What Are Biomedical Methods for Migraine ?
Biomedical methods for treating migraines involve medical and pharmacological approaches aimed at preventing, alleviating, or managing migraine symptoms. These methods often include medications and medical interventions designed to target the underlying causes or mechanisms of migraines. Here are some common biomedical methods for migraine management:
- Pain Relief Medications: These medications are used to relieve the pain and symptoms of a migraine attack when it occurs. They include:
- Triptans: These drugs, such as sumatriptan and rizatriptan, work by constricting blood vessels and blocking pain pathways in the brain.
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): Over-the-counter NSAIDs like ibuprofen and prescription-strength versions can help alleviate pain and reduce inflammation associated with migraines.
- Acetaminophen: This pain reliever can be effective for some migraine sufferers, although it may not be as potent as other medications.
- Preventive Medications: These medications are taken regularly to reduce the frequency, severity, and duration of migraine attacks. They are typically prescribed to individuals with frequent and severe migraines. Preventive medications include:
- Beta-Blockers: Drugs like propranolol and metoprolol may be used to prevent migraines.
- Anticonvulsants: Certain antiepileptic drugs like topiramate (Topamax) and valproate may be prescribed as preventive measures.
- Antidepressants: Tricyclic antidepressants (e.g., amitriptyline) and selective serotonin reuptake inhibitors (SSRIs) can be effective in some cases.
- Calcitonin Gene-Related Peptide (CGRP) Inhibitors: Monoclonal antibodies targeting CGRP or its receptor are a newer class of preventive medications.
- Medications for Nausea and Vomiting: Migraine attacks can cause nausea and vomiting, and medications like metoclopramide and ondansetron may be used to manage these symptoms.
- Hormone Therapy: For individuals with menstrual migraines, hormonal therapies, such as birth control pills or hormone replacement therapy (HRT), can help regulate hormonal fluctuations that trigger migraines.
- Nerve Blocks: Injection of local anesthetics or steroids around specific nerves (e.g., occipital nerve blocks) can help alleviate migraine pain.
- Neurostimulation Devices: Implantable devices like occipital nerve stimulators or supraorbital nerve stimulators can provide electrical stimulation to targeted nerves to reduce migraine frequency and intensity.
- Botulinum Toxin (Botox) Injections: Botox injections can be administered to specific areas of the head and neck to prevent chronic migraines in some individuals.
- Intravenous (IV) Medications: In severe cases, intravenous medications, such as dihydroergotamine (DHE) or magnesium sulfate, may be used in emergency or hospital settings to treat intractable migraines.
- CGRP Monoclonal Antibodies: These newer medications, such as erenumab (Aimovig) and fremanezumab (Ajovy), are specifically designed to target the CGRP pathway, which is believed to play a role in migraine development.
- Other Medications: In some cases, other medications not originally developed for migraines may be prescribed off-label if they have shown effectiveness in preventing or managing migraine attacks.
The choice of biomedical treatment for migraines depends on several factors, including the frequency and severity of attacks, individual response to medications, and the presence of coexisting medical conditions. Migraine management often involves a combination of acute pain relief and preventive measures, and it should be tailored to the specific needs of each patient. Patients should work closely with healthcare providers or headache specialists to develop a personalized treatment plan for their migraines.
Pain Medications, Pain Relief, and Pain Management