What is chronic Pain ?
Chronic pain is a persistent or long-lasting pain that extends beyond the typical duration of an injury or illness, typically defined as lasting for at least 12 weeks or longer. Unlike acute pain, which serves as a warning signal for the body to address an injury or illness, chronic pain often continues even after the initial cause of the pain has healed.
Chronic pain can take various forms and affect different parts of the body. It may result from a wide range of underlying conditions, including but not limited to:
- Musculoskeletal Disorders: Conditions like osteoarthritis, rheumatoid arthritis, and fibromyalgia can lead to chronic joint and muscle pain.
- Neuropathic Pain: Nerve damage or dysfunction can cause neuropathic pain, which is often described as burning, tingling, or shooting pain. Conditions like diabetic neuropathy and post-herpetic neuralgia fall into this category.
- Chronic Headaches: Conditions such as migraines, tension-type headaches, and cluster headaches can lead to recurrent and long-lasting head pain.
- Chronic Back Pain: Issues with the spine, such as herniated discs, degenerative disc disease, or spinal stenosis, can cause persistent back pain.
- Chronic Pelvic Pain: Conditions like endometriosis or chronic prostatitis can lead to ongoing pain in the pelvic region.
- Central Sensitization: This is a process in which the central nervous system becomes hypersensitive to pain signals, resulting in pain amplification and widespread discomfort.
- Cancer-Related Pain: In some cases, cancer can cause chronic pain as it progresses or following treatments like surgery, radiation, or chemotherapy.
- Injuries: Severe injuries or trauma, such as fractures, may result in chronic pain that persists long after the initial injury has healed.
- Autoimmune Diseases: Conditions like lupus or multiple sclerosis can cause chronic pain as part of their symptom profile.
What Is the Reasons of Chronic Pain ?
Chronic pain can have various underlying causes, and it often results from a complex interplay of factors. Chronic pain can originate from a variety of sources. Frequently, age-related changes can impact the bones and joints, leading to persistent pain. Additionally, nerve damage and improperly healed injuries are common contributors.
Some common reasons for chronic pain include:
- Injury or Trauma: Chronic pain can develop as a result of an injury, such as a fracture, sprain, or surgery. In some cases, the pain persists long after the initial injury has healed due to nerve damage or other factors.
- Underlying Medical Conditions: Many chronic medical conditions can lead to chronic pain. These include:
- Arthritis: Conditions like osteoarthritis and rheumatoid arthritis can cause persistent joint pain.
- Neurological Disorders: Conditions like multiple sclerosis or diabetic neuropathy can result in chronic neuropathic pain.
- Fibromyalgia: A disorder characterized by widespread musculoskeletal pain and tenderness.
- Inflammatory Bowel Disease: Conditions like Crohn’s disease and ulcerative colitis can cause abdominal pain.
- Endometriosis: A condition in which tissue similar to the lining of the uterus grows outside the uterus, leading to chronic pelvic pain.
- Chronic Headaches: Migraines, tension-type headaches, and cluster headaches can result in recurrent and long-lasting head pain.
- Nerve Pain: Damage or dysfunction of the nerves can cause chronic pain. Conditions like sciatica, post-herpetic neuralgia (shingles pain), or trigeminal neuralgia fall into this category.
- Central Sensitization: This is a process in which the central nervous system becomes hypersensitive to pain signals, leading to pain amplification and widespread discomfort. It can result from conditions like fibromyalgia and complex regional pain syndrome (CRPS).
- Psychological Factors: Psychological conditions like depression, anxiety, and post-traumatic stress disorder can worsen or contribute to chronic pain. This is often referred to as psychogenic pain or pain related to emotional factors.
- Autoimmune Diseases: Conditions like lupus or Sjögren’s syndrome can cause chronic pain as part of their symptom profile.
- Cancer: Advanced stages of cancer can lead to chronic pain due to tumor growth, compression of nerves, or the side effects of cancer treatments.
- Post-Surgical Pain: Some individuals experience chronic pain following surgical procedures. This is known as post-surgical chronic pain and can result from nerve damage, scar tissue formation, or other factors.
- Lifestyle and Behavioral Factors: Chronic pain can be exacerbated or perpetuated by lifestyle factors, such as poor posture, lack of exercise, or unhealthy diet.
- Genetic Factors: In some cases, a person’s genetic makeup can predispose them to conditions associated with chronic pain, such as certain types of arthritis.
Certain types of chronic pain may have multiple underlying causes. Take back pain, for instance; it can result from a singular factor or a combination of elements, including:
- Prolonged periods of poor posture.
- Incorrect techniques for lifting and carrying heavy objects.
- Excess weight, which places added stress on the back and knees.
- Congenital conditions like spinal curvature.
- Traumatic injuries.
- The use of high heels.
- Sleeping on an unsupportive mattress.
- Cases where there is no apparent physical cause.
- The natural aging process of the spine, involving degenerative changes.
Diseases can also serve as the underlying source of chronic pain. Conditions like rheumatoid arthritis, osteoarthritis, and fibromyalgia are recognized as common culprits. However, persistent pain may also arise from ailments such as cancer, multiple sclerosis, stomach ulcers, AIDS, or gallbladder disease.
Nevertheless, these conditions often require a more thorough examination.
Treating pain without identifying its cause presents a common challenge in medicine. For instance, many individuals mistakenly regard a headache as a standalone condition when, in reality, it serves as a symptom that may signal a more significant underlying issue.
Why Is It Important to Find the Reasons of Chronic Pain ?
It is important to find the reasons for chronic pain for several significant reasons:
- Proper Treatment: Understanding the underlying causes of chronic pain is crucial for effective treatment. Different conditions require different approaches to manage or alleviate pain. Accurate diagnosis allows healthcare professionals to tailor treatments that target the root cause, which can lead to better pain relief.
- Preventing Progression: Identifying the reasons behind chronic pain can help prevent the condition from worsening. If left untreated, certain medical conditions that cause chronic pain can progress and lead to further complications or permanent damage. Early intervention can mitigate this risk.
- Quality of Life: Chronic pain can significantly affect a person’s quality of life, often leading to physical and emotional distress, disability, and limitations in daily activities. Discovering the cause can help develop a comprehensive management plan that can improve a person’s overall well-being and functionality.
- Psychological Well-Being: Chronic pain is often associated with mental health issues, such as anxiety and depression. Knowing the cause of pain can reduce uncertainty and stress, and addressing both the physical and emotional aspects of pain can improve a person’s mental health.
- Cost-Effective Care: Identifying the underlying reasons for chronic pain can lead to more cost-effective healthcare. Targeted treatments are generally more efficient and can reduce the need for unnecessary or ineffective interventions, potentially saving both time and money.
- Patient Satisfaction: When patients understand the cause of their chronic pain and receive tailored treatment, they are more likely to be satisfied with their healthcare experience. Effective management can enhance patient trust in the healthcare system and improve overall satisfaction.
- Preventing Opioid Dependency: In cases of chronic pain, it is essential to find the root cause to avoid overreliance on opioid pain medications. Opioid addiction is a significant concern, and addressing the underlying pain condition can lead to alternative treatments that reduce the need for these potentially addictive medications.
- Improved Long-Term Outcomes: Finding the cause of chronic pain allows for long-term management and planning. It enables healthcare providers to offer guidance and strategies for maintaining or improving the patient’s condition over time.
Recurring headaches, migraines, joint pain, muscle aches, back problems: these are just some of the things that send us straight to the painkillers.

It starts with identifying exactly what the pain is.
How Many Types of Chronic Pain Are there ?
Chronic pain can be categorized into various types based on its underlying causes, location, and characteristics. While the following list is not exhaustive, it provides an overview of some common types of chronic pain:
- Nociceptive Pain: This type of pain results from the activation of pain receptors in response to tissue damage or inflammation. It can be further classified into two subtypes:
- Somatic Pain: Arising from the bones, muscles, or connective tissues. Examples include osteoarthritis and muscle strains.
- Visceral Pain: Originating from internal organs, often due to conditions like irritable bowel syndrome or kidney stones.
- Neuropathic Pain: Neuropathic pain is caused by damage or dysfunction in the nervous system. It is often described as burning, tingling, or shooting pain and can be associated with conditions such as diabetic neuropathy, post-herpetic neuralgia, or sciatica.
- Musculoskeletal Pain: This category includes chronic pain that affects the muscles, bones, tendons, and ligaments. Conditions like fibromyalgia, chronic low back pain, and myofascial pain syndrome fall into this category.
- Chronic Headaches: Chronic headaches are persistent and can include various types such as migraines, tension-type headaches, and cluster headaches.
- Central Sensitization: Central sensitization is a condition in which the central nervous system becomes hypersensitive to pain signals, leading to widespread and amplified pain. It is associated with conditions like fibromyalgia and complex regional pain syndrome (CRPS).
- Pelvic Pain: Chronic pelvic pain can be due to conditions such as endometriosis, interstitial cystitis, or chronic prostatitis.
- Inflammatory Pain: This type of pain is linked to inflammatory conditions like rheumatoid arthritis and ankylosing spondylitis.
- Cancer-Related Pain: Advanced stages of cancer can lead to chronic pain due to tumor growth, nerve compression, or the side effects of cancer treatments.
- Post-Surgical Pain: Some individuals experience chronic pain following surgical procedures, often resulting from complications, nerve damage, or scar tissue formation.
- Psychogenic Pain: Psychological factors, such as depression, anxiety, or stress, can exacerbate or contribute to chronic pain. This is often referred to as psychogenic pain.
- Mixed Pain: Many individuals with chronic pain may experience a combination of nociceptive and neuropathic pain, making diagnosis and treatment more complex.
- Medication-Induced Pain: Long-term use of certain medications, including opioids, can lead to pain known as opioid-induced hyperalgesia.
- Unknown or Idiopathic Pain: In some cases, the exact cause of chronic pain remains unclear, and it is referred to as idiopathic pain.
It’s important to note that individuals may experience chronic pain in unique ways, and pain management approaches should be tailored to the specific type and underlying causes of pain. Accurate diagnosis and an individualized treatment plan are essential for effectively managing chronic pain.
How to Treat Chronic Pain ?
The treatment of chronic pain is often a complex and multidisciplinary process that depends on the underlying cause of the pain and the individual’s specific needs. Here are some common approaches to treating chronic pain:
- Diagnosis: The first step in treating chronic pain is to identify the underlying cause. This may involve a thorough medical evaluation, including physical examinations, imaging studies, and sometimes specialized tests. Understanding the source of the pain is crucial for developing an effective treatment plan.
- Medications: Medications are often a part of pain management. The type of medication prescribed depends on the cause and nature of the pain. Some common categories of pain medications include:
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): These drugs can help reduce pain and inflammation.
- Opioids: In some cases, strong pain medications like opioids may be prescribed, but their use is often limited due to the risk of dependence and other side effects.
- Antidepressants: Certain antidepressants, such as tricyclic antidepressants and selective serotonin-norepinephrine reuptake inhibitors (SNRIs), can help with chronic pain, particularly neuropathic pain.
- Anticonvulsants: Medications like gabapentin and pregabalin are effective for neuropathic pain.
- Muscle Relaxants: These may be prescribed for pain associated with muscle tension or spasms.
- Topical Analgesics: Creams or patches containing pain-relieving medications can be applied directly to the painful area.
- Physical Therapy: Physical therapists can develop exercise and stretching routines to improve mobility and reduce pain. They may also use techniques like manual therapy and modalities like heat or cold therapy.
- Occupational Therapy: Occupational therapists can help individuals with chronic pain learn how to perform daily tasks with less discomfort. They may recommend adaptive tools or ergonomic modifications.
- Psychological Support: Chronic pain can lead to depression, anxiety, and stress. Therapy, such as cognitive-behavioral therapy (CBT), can help individuals cope with the emotional aspects of chronic pain.
- Interventional Procedures: In some cases, injections or nerve blocks may be used to target the source of the pain directly. These procedures can provide temporary or long-lasting relief.
- Surgery: For specific conditions, surgery may be necessary to correct the underlying problem causing chronic pain. Surgical interventions are typically considered after other treatments have been exhausted.
- Complementary and Alternative Therapies: Some individuals find relief through complementary therapies such as acupuncture, chiropractic care, massage, or biofeedback.
- Lifestyle Modifications: Lifestyle changes, including maintaining a healthy diet, regular exercise, and stress management, can help reduce the impact of chronic pain.
- Pain Management Programs: These are specialized programs offered by pain clinics that provide a comprehensive, multidisciplinary approach to chronic pain treatment. They often combine various therapies and support services.
It’s important for individuals with chronic pain to work closely with their healthcare providers to develop a personalized pain management plan. This plan should take into account the specific type of pain, its severity, and any underlying medical conditions. It’s also essential to communicate openly with healthcare providers to monitor the effectiveness of treatment and make adjustments as needed.
What Kinds of Pains Can Be Treated by Gabapentin ?
Gabapentin is a medication primarily used to treat certain types of pain, particularly neuropathic pain, and is also used to manage seizures and some other medical conditions. The pain conditions that can be treated by gabapentin include:
- Neuropathic Pain: Gabapentin is often prescribed to relieve neuropathic pain, which results from damage or dysfunction of the nerves. This type of pain is characterized by burning, shooting, or tingling sensations. Conditions such as diabetic neuropathy, post-herpetic neuralgia (shingles pain), and peripheral neuropathy may respond well to gabapentin.
- Chronic Pain: Gabapentin can be used to manage various types of chronic pain, including musculoskeletal pain, such as fibromyalgia, and certain types of chronic back pain.
- Migraines and Chronic Headaches: Some individuals with chronic migraines or other chronic headache disorders may find relief with gabapentin.
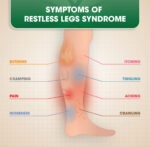
- Restless Legs Syndrome: Gabapentin can be used to alleviate the discomfort associated with restless legs syndrome, a condition characterized by an irresistible urge to move the legs, often accompanied by uncomfortable sensations.
- Post-Surgical Pain: Gabapentin is sometimes prescribed after surgery to help manage post-operative pain, particularly when nerve pain is a concern.
- Epilepsy and Seizure Disorders: Gabapentin is an anticonvulsant and is effective in controlling seizures in individuals with epilepsy.
It’s important to note that gabapentin is not effective for all types of pain. While it can be a valuable option for many individuals with neuropathic or chronic pain, its efficacy varies from person to person. Additionally, gabapentin is not typically used for acute or short-term pain relief.
The appropriate use of gabapentin should be determined by a healthcare professional who can assess the specific pain condition and determine the most suitable treatment plan, including the dosage and duration of gabapentin therapy.
Pain Medications, Pain Relief, and Pain Management