Osteoarthritis (AH-stee-oh-ar-THREYE-tis) is the most common type of arthritis and is seen especially among older people. Sometimes it is called degenerative joint disease. Osteoarthritis mostly affects cartilage (KAR-til-uj), the hard but slippery tissue that covers the ends of bones where they meet to form a joint. Healthy cartilage allows bones to glide over one another. It also absorbs energy from the shock of physical movement.

In osteoarthritis, the surface layer of cartilage breaks and wears away. This allows bones under the cartilage to rub together, causing pain, swelling, and loss of motion of the joint. Over time, the joint may lose its normal shape. Also, small deposits of bone—called osteophytes or bone spurs—may grow on the edges of the joint. Bits of bone or cartilage can break off and float inside the joint space. This causes more pain and damage.
Osteoarthritis is by far the most common type of arthritis, and the percentage of people who have it grows higher with age. An estimated 27 million Americans age 25 and older have osteoarthritis.
Although osteoarthritis becomes more common with age, younger people can develop it, usually as the result of a joint injury, a joint malformation, or a genetic defect in joint cartilage. Both men and women have the disease. Before age 45, more men than women have osteoarthritis; after age 45, it is more common in women. It is also more likely to occur in people who are overweight and in those with jobs that stress particular joints.
What is osteoarthritis (OA)?
Osteoarthritis (OA) is the most common form of arthritis. Some people call it degenerative joint disease or “wear and tear” arthritis. It occurs most frequently in the hands, hips, and knees.
With OA, the cartilage within a joint begins to break down and the underlying bone begins to change. These changes usually develop slowly and get worse over time. OA can cause pain, stiffness, and swelling. In some cases it also causes reduced function and disability; some people are no longer able to do daily tasks or work.
What are the signs and symptoms of OA?
- Pain. Affected joints might hurt during or after movement.
- Stiffness. Joint stiffness might be most noticeable upon awakening or after being inactive.
- Tenderness. Your joint might feel tender when you apply light pressure to or near it.
- Loss of flexibility. You might not be able to move your joint through its full range of motion.
- Grating sensation. You might feel a grating sensation when you use the joint, and you might hear popping or crackling.
- Bone spurs. These extra bits of bone, which feel like hard lumps, can form around the affected joint.
- Swelling. This might be caused by soft tissue inflammation around the joint.
How many people have OA?
OA affects over 32.5 million US adults.
What causes OA?
OA is caused by damage or breakdown of joint cartilage between bones.
Osteoarthritis occurs when the cartilage that cushions the ends of bones in your joints gradually deteriorates. Cartilage is a firm, slippery tissue that enables nearly frictionless joint motion. Eventually, if the cartilage wears down completely, bone will rub on bone.
Osteoarthritis has often been referred to as a “wear and tear” disease. But besides the breakdown of cartilage, osteoarthritis affects the entire joint. It causes changes in the bone and deterioration of the connective tissues that hold the joint together and attach muscle to bone. It also causes inflammation of the joint lining.
What are the risk factors for OA?
- Joint injury or overuse—Injury or overuse, such as knee bending and repetitive stress on a joint, can damage a joint and increase the risk of OA in that joint.
- Age—The risk of developing OA increases with age.
- Gender—Women are more likely to develop OA than men, especially after age 50.
- Obesity—Extra weight puts more stress on joints, particularly weight-bearing joints like the hips and knees. This stress increases the risk of OA in that joint. Obesity may also have metabolic effects that increase the risk of OA.
- Genetics—People who have family members with OA are more likely to develop OA. People who have hand OA are more likely to develop knee OA.
- Race— Some Asian populations have lower risk for OA.
How is OA diagnosed?
A doctor diagnoses OA through a review of symptoms, physical examination, X-rays, and lab tests.
A rheumatologist, a doctor who specializes in arthritis and other related conditions, can help if there are any questions about the diagnosis.
During the physical exam, your doctor will check your affected joint for tenderness, swelling, redness and flexibility.
Imaging tests
To get pictures of the affected joint, your doctor might recommend:
- X-rays. Cartilage doesn’t show up on X-ray images, but cartilage loss is revealed by a narrowing of the space between the bones in your joint. An X-ray can also show bone spurs around a joint.
- Magnetic resonance imaging (MRI). An MRI uses radio waves and a strong magnetic field to produce detailed images of bone and soft tissues, including cartilage. An MRI isn’t commonly needed to diagnose osteoarthritis but can help provide more information in complex cases.
Lab tests
Analyzing your blood or joint fluid can help confirm the diagnosis.
- Blood tests. Although there’s no blood test for osteoarthritis, certain tests can help rule out other causes of joint pain, such as rheumatoid arthritis.
- Joint fluid analysis. Your doctor might use a needle to draw fluid from an affected joint. The fluid is then tested for inflammation and to determine whether your pain is caused by gout or an infection rather than osteoarthritis.
How is OA treated?
There is no cure for OA, so doctors usually treat OA symptoms with a combination of therapies, which may include the following:
- Increasing physical activity
- Physical therapy with muscle strengthening exercises
- Weight loss
- Medications, including over-the-counter pain relievers and prescription drugs
- Supportive devices such as crutches or canes
- Surgery (if other treatment options have not been effective)
In addition to these treatments, people can gain confidence in managing their OA with self-management strategies. These strategies help reduce pain and disability so people with osteoarthritis can pursue the activities that are important to them. These five simple and effective arthritis management strategies can help.
Osteoarthritis can’t be reversed, but treatments can reduce pain and help you move better.
Medications
Medications that can help relieve osteoarthritis symptoms, primarily pain, include:
- Acetaminophen. Acetaminophen (Tylenol, others) has been shown to help some people with osteoarthritis who have mild to moderate pain. Taking more than the recommended dose of acetaminophen can cause liver damage.
- Nonsteroidal anti-inflammatory drugs (NSAIDs). Over-the-counter NSAIDs, such as ibuprofen (Advil, Motrin IB, others) and naproxen sodium (Aleve, others), taken at the recommended doses, typically relieve osteoarthritis pain. Stronger NSAIDs are available by prescription.NSAIDs can cause stomach upset, cardiovascular problems, bleeding problems, and liver and kidney damage. NSAIDs as gels, applied to the skin over the affected joint, have fewer side effects and may relieve pain just as well.
- Duloxetine (Cymbalta). Normally used as an antidepressant, this medication is also approved to treat chronic pain, including osteoarthritis pain.
Alternative medicine
Complementary and alternative medicine treatments that have shown promise for osteoarthritis include:
- Acupuncture. Some studies indicate that acupuncture can relieve pain and improve function in people who have knee osteoarthritis. During acupuncture, hair-thin needles are inserted into your skin at precise spots on your body.
- Glucosamine and chondroitin. Studies have been mixed on these nutritional supplements. A few have found benefits for people with osteoarthritis, while most indicate that these supplements work no better than a placebo. Glucosamine and chondroitin can interact with blood thinners such as warfarin and cause bleeding problems.
- Avocado-soybean unsaponifiables. This nutritional supplement — a mixture of avocado and soybean oils — is widely used in Europe to treat knee and hip osteoarthritis. It acts as an anti-inflammatory, and some studies have shown it can slow or even prevent joint damage.
- Omega-3 fatty acids. Omega-3s, found in fatty fish and fish oil supplements, might help relieve pain and improve function.
Physical Activity for Arthritis
Some people are concerned that physical activity will make their arthritis worse, but joint-friendly physical activity can actually improve arthritis pain, function, and quality of life.
Osteoarthritis, the most prevalent form of arthritis, is a persistent and progressive ailment characterized by the deterioration of the protective cartilage that normally covers the ends of bones where they articulate in a joint.
Dr. Katz explains, “This condition gradually erodes joint cartilage, causing the forces that are typically absorbed by the cartilage to be transferred to the bone, which contains pain-sensitive nerve fibers.” This cartilage breakdown can lead to pain, swelling, inflammation, and limitations in physical activity.
Osteoarthritis primarily afflicts the knees, hips, and lower back, and its incidence increases with age. However, various factors can heighten an individual’s susceptibility, including a family history of the ailment, prior injuries, and excess body weight.
Regrettably, there is no cure for osteoarthritis. Nonsteroidal anti-inflammatory drugs like ibuprofen (Advil, Motrin), naproxen (Aleve), or aspirin can provide temporary relief from pain and inflammation. In some cases, steroid injections may offer short-term respite.
An alternative approach to symptom management involves physical activity. Dr. Katz emphasizes, “Exercise may not replace lost cartilage or necessarily halt its natural degeneration, but it plays a crucial role by strengthening bones and the surrounding muscles, thereby safeguarding affected joints from excessive stress and enabling them to function more effectively.”
How can I manage OA and improve my quality of life?
CDC’s Arthritis Program recommends five self-management strategies for managing arthritis and its symptoms.
- Learn self-management skills. Join a self-management education class, which helps people with arthritis and other chronic conditions—including OA—understand how arthritis affects their lives and increase their confidence in controlling their symptoms and living well. Learn more about the CDC-recommended self-management education programs.
- Get physically active. Experts recommend that adults engage in 150 minutes per week of at least moderate physical activity. Every minute of activity counts, and any activity is better than none. Moderate, low impact activities recommended include walking, swimming, or biking. Regular physical activity can also reduce the risk of developing other chronic diseases such as heart disease, stroke, and diabetes. Learn more about physical activity for arthritis.
- Go to effective physical activity programs. For people who worry that physical activity may make OA worse or are unsure how to exercise safely, participation in physical activity programs can help reduce pain and disability related to arthritis and improve mood and the ability to move. Classes take place at local Ys, parks, and community centers. These classes can help people with OA feel better. Learn more about CDC-recommended physical activity programs.
- Talk to your doctor. You can play an active role in controlling your arthritis by attending regular appointments with your health care provider and following your recommended treatment plan. This is especially important if you also have other chronic conditions, like diabetes or heart disease.
- Lose weight. For people who are overweight or obese, losing weight reduces pressure on joints, particularly weight bearing joints like the hips and knees. Reaching or maintaining a healthy weight can relieve pain, improve function, and slow the progression of OA.
- Protect your joints. Joint injuries can cause or worsen arthritis. Choose activities that are easy on the joints like walking, bicycling, and swimming. These low-impact activities have a low risk of injury and do not twist or put too much stress on the joints. Learn more about how to exercise safely with arthritis.
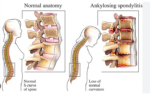
Osteoarthritis is the most common form of arthritis. It causes pain, swelling, and reduced motion in your joints. It can occur in any joint, but usually it affects your hands, knees, hips or spine.
Osteoarthritis breaks down the cartilage in your joints. Cartilage is the slippery tissue that covers the ends of bones in a joint. Healthy cartilage absorbs the shock of movement. When you lose cartilage, your bones rub together. Over time, this rubbing can permanently damage the joint.
Risk factors for osteoarthritis include
- Being overweight
- Getting older
- Injuring a joint
There is no specific test for osteoarthritis. Most doctors use several methods, including medical history, a physical exam, x-rays, or lab tests.
Treatments include exercise, medicines, and sometimes surgery.
Preventing Osteoarthritis Pain Through Exercise
Exercise not only has the potential to mitigate the progression of osteoarthritis but may also reduce the likelihood of developing the condition in the first place. A study examining the relationship between running and the risk of hip or knee osteoarthritis revealed that merely 3.5% of individuals who engaged in regular running for exercise eventually developed knee or hip osteoarthritis, as opposed to 10% of those who remained inactive.
Another study uncovered encouraging results among individuals with mild knee osteoarthritis or those at higher-than-average risk for the disease. It demonstrated that individuals who maintained an average of nearly 7,000 steps per day, equivalent to more than three miles of walking, did not experience additional cartilage loss over a span of two years.
These findings emphasize the substantial benefits of physical activity in preventing and managing the pain associated with osteoarthritis. Exercise serves as a valuable tool in preserving joint health and quality of life for those at risk or already affected by this condition.
Pain Medications, Pain Relief, and Pain Management