A migraine headache is a form of vascular headache. Migraine headache is caused by vasodilatation (enlargement of blood vessels) that causes the release of chemicals from nerve fibers that coil around the large arteries of the brain.
Enlargement of these blood vessels stretches the nerves that coil around them and causes the nerves to release chemicals. The chemicals cause inflammation, pain, and further enlargement of the artery.
The increasing enlargement of the arteries magnifies the pain.

What is Migraine Headache ?
A migraine is a type of headache that typically causes intense, throbbing pain usually in one area of the head. People can experience migraines once a year to multiple times a week. A person is considered to have chronic migraines if they experience 15 or more headache days a month with eight of those days involving migraine headaches.
Migraines typically first start during a person’s teens to early twenties, but they can begin anytime from early childhood to late-adulthood.
A migraine usually has three stages: the period leading up to the headache (known as the premonitory or prodromal phase), the migraine itself (the headache phase), and the period following the headache (known as the postdromal phase).
The premonitory phase can start from several hours up to several days before the headache appears. In this phase, affected individuals can experience extreme tiredness (fatigue), concentration problems, and muscle stiffness in the neck. A wide variety of additional signs and symptoms can occur including excessive yawning, food cravings, irritability, depression, sensitivity to light, and nausea. About one-third of people with migraine experience a temporary pattern of neurological symptoms called an aura.
An aura typically develops gradually over a few minutes and lasts between 5 and 60 minutes. Auras commonly include temporary visual changes such as blind spots (scotomas), flashing lights, and zig-zagging lines of color. Additional features of aura can include numbness, difficulty with speech and language, episodes of extreme dizziness (vertigo), and double vision. During an aura, affected individuals might experience abnormal sensations including tingling or numbness, usually of the hands or mouth. An aura usually starts within one hour of the start of a migraine. In some cases, an aura can occur without a subsequent migraine.
In the headache phase, the pain may last from a few hours to a few days. Affected individuals tend to experience nausea, vomiting, dizziness, and sensitivity to light and sound in addition to headache. Some have changes in their vision or sensitivity to odors and touch.
The postdromal phase usually lasts a few hours but can linger for more than a day. In this phase, the headache pain is gone but individuals can experience fatigue, drowsiness, decreased energy, concentration problems, irritability, nausea, or sensitivity to light. Affected individuals may also have brief episodes of head pain when moving their head.
People with migraine, particularly women who have migraine with aura, have an increased risk of a type of stroke that is caused by a lack of blood flow to the brain ), but this is a rare occurrence.
There are many migraine disorders that usually include additional signs and symptoms. For example, familial hemiplegic migraine and sporadic hemiplegic migraine are characterized by migraine with associated temporary weakness that affects one side of the body (hemiparesis). Additionally, cyclic vomiting syndrome is a migraine disorder usually found in children that causes episodes of nausea and vomiting in addition to headaches.
Migraine attacks commonly activate the sympathetic nervous system in the body.
The sympathetic nervous system is often thought of as the part of the nervous system that controls primitive responses to stress and pain, the so-called “fight or flight” response, and this activation causes many of the symptoms associated with migraine attacks; for example, the increased sympathetic nervous activity in the intestine causes nausea, vomiting, and diarrhea.
The Types of Migrains
Migraine is a neurological condition that is characterized by recurrent headaches that are often accompanied by other symptoms, such as sensitivity to light, sound, and smells. There are several types of migraines, including:
- Migraine without aura: This is the most common type of migraine, and it does not have any warning signs or “aura” before the headache starts.
- Migraine with aura: This type of migraine is characterized by a warning sign or aura that occurs before the headache starts. Auras may include visual disturbances, such as seeing flashing lights or zigzag lines, or sensory changes, such as tingling in the hands or face.
- Chronic migraine: This is a type of migraine that occurs for 15 or more days per month for at least three months. Chronic migraine can be a difficult condition to manage and may require specialized treatment.
- Menstrual migraine: This type of migraine occurs in women during their menstrual cycle, and is thought to be caused by changes in hormone levels.
- Vestibular migraine: This type of migraine is associated with dizziness or vertigo and can be accompanied by visual disturbances, such as blurred vision.
- Hemiplegic migraine: This is a rare type of migraine that can cause temporary paralysis or weakness on one side of the body.
- Retinal migraine: This type of migraine is characterized by temporary vision loss or blindness in one eye.
It’s important to note that each person may experience migraines differently, and the symptoms and triggers may vary from person to person. If you experience migraines, it’s important to work with a healthcare professional to identify the type of migraine you have and develop an individualized treatment plan.
Symptoms of Migraine Headaches:
Migraine is a chronic condition with recurrent attacks. Most (but not all) migraine attacks are associated with headaches.
Migraine headaches usually are described as an intense, throbbing or pounding pain that involves one temple. (Sometimes the pain is located in the forehead, around the eye, or at the back of the head).
The pain usually is unilateral (on one side of the head), although about a third of the time the pain is bilateral (on both sides of the head).
The unilateral headaches typically change sides from one attack to the next. (In fact, unilateral headaches that always occur on the same side should alert the doctor to consider a secondary headache, for example, one caused by a brain tumor).
A migraine headache usually is aggravated by daily activities such as walking upstairs.
Nausea, vomiting, diarrhea, facial pallor, cold hands, cold feet, and sensitivity to light and sound commonly accompany migraine headaches. As a result of this sensitivity to light and sound, migraine sufferers usually prefer to lie in a quiet, dark room during an attack. A typical attack lasts between 4 and 72 hours.
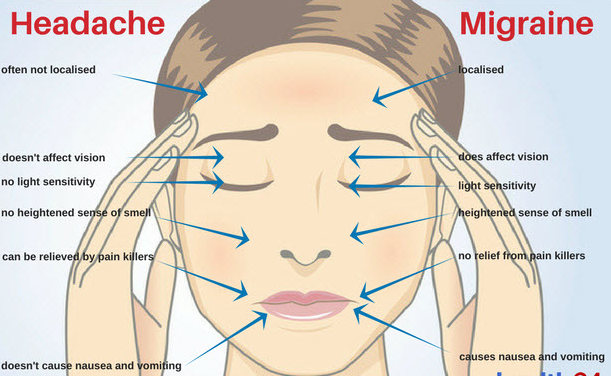
With or Without Aura?
The two most common types of migraine fall into two categories: migraine without aura and migraine with aura.
70-90% of people with migraine experience this type, with attacks lasting between 4 to 72 hours when not successfully treated. Attacks are irregular – they may occur several times a week, or just once a year.
Common symptoms include:
- A throbbing or pulsating pain on one side of the head
- Pain worsens when doing even everyday activities, like walking or climbing stairs
- Nausea, or vomiting
- May become sensitive to light (photophobia) and/or sounds (phonophobia)
With Aura
The term aura describes the neurological disturbances that can accompany a migraine. It happens to about 1 in 4 people affected by migraines, and each individual symptom during an aura may last 5-60 minutes. Aura usually occurs before the headache, but it may begin after the headache phase has started, or continue into the headache phase. It’s often a sign of an impending attack, although it is possible to experience an aura without an associated headache.
If you have a migraine with aura, you may experience all the symptoms of migraine without aura, plus these additional symptoms:
- Visual symptoms like seeing wavy lines, shapes, dots or flashes
- Blurry vision or blind spots
- Temporary loss of vision
- Tingling or numbness in your arms and legs
- Weakness on one side of the body
- Changes to your sense of smell, taste or touch
Aura can occur anywhere from once a year to several times a week. Aside from migraine with typical aura, there are other sub-types under the Migraine with aura category.
Symptoms associated with hemiplegic migraines may last for several days
There are 2 types of hemiplegic migraine: familial, which runs in families, and sporadic (occurs randomly). If you experience any of these symptoms, or suspect you may suffer from hemiplegic migraine, see your doctor for more information and a treatment plan.
Retinal Migraine Symptoms
This form of aura migraine is very rare. It involves visual disturbances, however unlike other migraines that may affect both eyes, retinal migraine affects only one eye. Most often it occurs on the same side as the migraine headache.
The reversible visual symptoms may be as short as a few seconds, but normally last several minutes to an hour, and may be followed by a typical migraine headache. In rare cases, the visual loss in one eye can last hours, days and even weeks.
Retinal Migraines only affect one eye
Disturbances to one eye include:
- Flashing lights, zigzag patterns, coloured streaks, halos and diagonal lines
- Vision losses such as blurring, blind spots, black dots, or partial or complete blindness
- Tunnel vision (loss of peripheral vision)
Because loss of vision in one eye isn’t always related to migraine and may be caused by some other underlying serious condition, it’s important to see your doctor right away for treatment.
The term ocular migraine is often used to describe retinal migraine or sometimes even migraine with aura, and some doctors still use this term, though it is not recognized in the ICHD-3 classification system.
The Causes of Migraine Headaches
Migraines are thought to occur when blood flow in the brain is altered and certain nerves in the brain send abnormal pain signals throughout the head. These signals trigger the release of various brain chemicals in the brain, which leads to inflammation, particularly of blood vessels and the membrane that covers the brain and spinal cord (meninges). This inflammation causes many of the signs and symptoms of a migraine, including the throbbing pain, nausea, and sensory sensitivities. However, it is unclear what leads to the abnormal nerve signaling.
Auras are thought to be caused by abnormal nerve signaling and associated changes in blood flow that spread across the brain. Additionally, the release of large amounts of the neurotransmitter glutamate is thought to contribute to aura. The causes of these imbalances are unclear.
Migraines result from a combination of genetic, environmental, and lifestyle factors, some of which have not been identified. Variations in many genes have been found to be associated with the development of migraines with or without aura. These genes likely have varying degrees of impact among affected individuals. Most of the associated genes are active in the muscles that surround blood vessels within the brain. These genes help regulate blood flow by controlling the narrowing and expansion of blood vessels. Many variants likely disrupt blood flow in the brain, which can contribute to developing migraines. Changes in blood flow in the brain or in the balance between vascular injury and repair (vascular homeostasis) also likely underlie the increased risk of stroke in people with migraines. Variants in genes that regulate levels of glutamate or the activity (excitability) of certain nerve cells in the brain have also been found in people with migraines.
Nongenetic factors also play a critical role in developing a migraine. Migraine headaches can be triggered by skipping meals, caffeine or alcohol overuse, certain foods, poor sleep, emotional stress, hormonal changes, or minor head trauma. Excessive use of pain relief medications can also trigger or worsen migraines.
Migraine Headaches Treated:
Acetaminophen reduces pain and fever by acting on pain centers in the brain. Acetaminophen is well tolerated and generally is considered easier on the stomach than NSAIDs. However, acetaminophen can cause severe liver damage in high (toxic) doses or if used on a regular basis over extended periods of time. In individuals who regularly consume moderate or large amounts of alcohol, acetaminophen can cause serious damage to the liver in lower doses that usually are not toxic. Acetaminophen also can damage the kidneys when taken in large doses. Therefore, acetaminophen should not be taken more frequently or in larger doses than recommended on the package label.
NSAIDS
Examples of non-aspirin NSAIDs are ibuprofen (Advil, Nuprin, Motrin IB, and Medipren) and naproxen (Aleve). Some NSAIDs are available by prescription only. Prescription NSAIDs are usually prescribed to treat arthritis and other inflammatory conditions such as bursitis, tendonitis, etc. The difference between OTC and prescription NSAIDs usually is the amount of the active ingredient contained in each pill. For example, OTC naproxen (Aleve) contains 220 mg of naproxen per pill, whereas prescription naproxen (Naprosyn) contains 375 or 500 mg of naproxen per pill.
NSAIDs relieve pain by reducing the inflammation that causes the pain (they are called nonsteroidal antiinflammatory drugs or NSAIDs because they are different from corticosteroids such as prednisone, prednisolone, and cortisone which also reduce inflammation). Corticosteroids, though valuable in reducing inflammation, have predictable and potentially serious side effects, especially when used long-term. Their full effects also require hours or days. NSAIDs do not have the same side effects that corticosteroids have and their onset of action is faster.
Aspirin, Aleve, Motrin, and Advil all are NSAIDs and are similarly effective in relieving pain and fever. The main difference between aspirin and non-aspirin NSAIDs is their effect on platelets, the small particles in blood that cause blood clots to form. Aspirin prevents the platelets from forming blood clots. Therefore, aspirin can increase bleeding by preventing blood from clotting though it also can be used therapeutically to prevent clots from causing heart attacks and strokes. The non-aspirin NSAIDs also have antiplatelet effects, but their antiplatelet action does not last as long as aspirin, i.e. hours rather than days.
Amitriptyline (Elavil) is an antidepressant. The dosing ranges from once a day up to four times a day. It belongs to a group of antidepressants called tricyclics. Drowsiness and sleepiness are very common with this group, so your doctor may recommend taking it at bedtime.
Divalproex sodium extended-release (Depakote ER) is an anticonvulsant. You take the extended-release tablet once a day. Taking it with food can help prevent stomach upset.
Eletriptan (Relpax) is a triptan. It is a tablet you take at the onset of your migraine symptoms. For triptans, your doctor will tell you how many tablets you can take in a 24 hour period.
Metoprolol (Lopressor, Toprol XL) is a beta blocker. It comes in both an immediate-release and an extended-release form.
Propranolol extended-release (Inderal, Inderal LA, Inderal XL) is another beta blocker. It comes in several forms, each with their own dosing. Talk with your doctor or pharmacist about how to take your medicine.
Rizatriptan (Maxalt) is a triptan you use at the onset of symptoms. It comes as a tablet and a disintegrating tablet, which melts in your mouth without water.
Sumatriptan (Imitrex) is another triptan. It comes in several forms, including a tablet, injection, and nasal spray.
Topiramate (Topamax, Trokendi XR) is an anticonvulsant. It comes in a regular-release tablet and an extended-release capsule. You can take either kind with or without food.
Venlafaxine (Effexor, Effexor XR) is an antidepressant. You take both the tablet and the extended-release capsule with food. Stomach upset, headache, and appetite loss are common side effects.
Zolmitriptan (Zomig) is another triptan. It comes as a tablet, disintegrating table, and nasal spray.
OnabotulinumtoxinA (Botox) is a botulinum toxin that, when injected into areas of the face and scalp, can prevent the brain’s pain response from activating. This stops migraine attacks before they occur.
Erenumab (Aimovig) is a CGRP blocker. It’s given by self-injection once a month.
Find powerful herbal remedies
Home Remedies for Migraine Relief
Aspirin, acetaminophen, and caffeine also are available combined in OTC analgesics for the treatment of headaches including migraine. Examples of such combination analgesics are Pain-aid, Excedrin, Fioricet, and Fiorinal.
Finding an effective analgesic or analgesic combination often is a process of trial and error because individuals respond differently to different analgesics. In general, a person should use the analgesic that has worked in the past. This will increase the likelihood that an analgesic will be effective and decrease the risk of side effects.
The Preventive Treatment of Migraine
The main classes of preventive treatment migraine drugs include:
- Antidepressants also balance brain chemicals that play a role in migraine. Side effects vary depending on the drug.
- Anticonvulsants are drugs that treat seizures through various effects on the brain. Common side effects include sleepiness and weight changes.
- Beta blockers. Drugs in this class commonly treat high blood pressure. Dizziness, fatigue and nausea are common side effects.
- Botulinum toxins are injected to prevent migraine in people with 15 or more headache days each month. Common side effects include headache, neck pain, and pain at the injection site.
- Monoclonal antibody CGRP blockers are the first class of drugs specifically produced to prevent migraines. They block a molecule thought to instigate migraine and increase migraine pain and intensity. This drug is injected under the skin. Common side effects include redness at the injection site, constipation, or muscle spasms or cramps.
Gabapentin for the Prophylaxis of Episodic Migraine in Adults
Clinical Question
Does gabapentin (Neurontin) help prevent episodic migraine?
Evidence-Based Answer
Gabapentin does not decrease the frequency of migraine headaches and is not recommended for prophylactic therapy. (Strength of Recommendation: B, based on inconsistent or limited-quality patient-oriented evidence.)
Practice Pointers
Worldwide, migraine has a lifetime prevalence of 18% in women and 10% in men. Therapeutic options are usually divided into prophylactic and abortive. Avoidance of triggers may be beneficial. Effective prophylaxis can range from acupuncture to medications such as propranolol, topiramate (Topamax), and valproic acid (Depakene), all of which have shown consistent positive benefit in systematic reviews.
Previously published systematic reviews by these same authors gave cautious support for the use of gabapentin for migraine prophylaxis based on poor-quality evidence. However, new data from not-yet-published industry-sponsored trials of gabapentin for migraine have come to light during litigation against the drug manufacturer. These data have led the authors to change their conclusion based on the results of five studies involving 1,009 patients.
Four trials with a total of 351 patients compared gabapentin in a dosage of 900 to 2,400 mg per day with placebo. The meta-analysis found no significant reduction in the frequency of migraine headache (mean difference in the number of headaches = −0.44; 95% confidence interval, −1.43 to 0.56). Pooled results of two studies with 235 patients comparing the proportion of responders (at least 50% improvement in frequency of headaches) between those treated with up to 2,400 mg of gabapentin vs. placebo failed to show a difference (odds ratio = 1.59; 95% confidence interval, 0.57 to 4.46). One study analyzed prophylactic use of the prodrug gabapentin enacarbil (Horizant) titrated up to 3,000 mg daily and failed to find any benefit.
Patients taking gabapentin often reported adverse effects, most commonly dizziness (number needed to harm [NNH] = 7), drowsiness (NNH = 9), and abnormal thinking (NNH = 20).
According to the Quality Standards Subcommittee of the American Academy of Neurology and the American Headache Society, prophylaxis should be offered to anyone whose daily activities are severely impaired, or when acute drug treatment is inadequate. The antiepileptic drugs topiramate and valproic acid are considered first-line prophylactic agents. However, the guidelines state that the evidence is inadequate to recommend the use of gabapentin for migraine prevention. Because gabapentin is not effective and commonly causes adverse effects, family physicians should consider alternatives when offering prophylaxis for migraine headache.
Pain Medications, Pain Relief, and Pain Management