Migraines Are a Very Common Condition and Can Be Severely Debilitating
Migraines are a very common condition, with 15.3% of Americans aged 18 years or older reporting a migraine or severe headache in the previous 3 months,[1] a figure that has remained stable for almost two decades. Migraines can be severely debilitating and are considered one of the main causes of disability worldwide. In one study among patients with migraines in the United States, more than half reported severe impairment in activity, the need for bed rest, and/or reduced work or school productivity due to migraines.
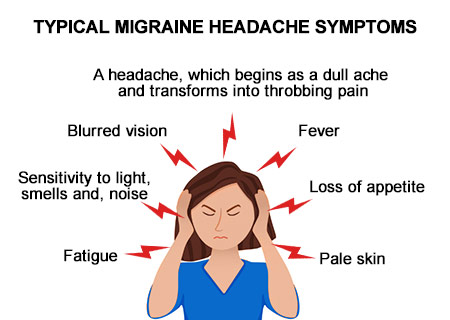
If you suffer from debilitating migraines, then you know how painful and limiting the neurological disorder can be. You’ve been forced to miss important events due to that pulsating pain and ever-present nausea. You’ve even had to adjust to lifestyle changes, making sure you get just enough sleep—not too little and not too much. You take the medicines regularly, both the preventative type and the kind that helps you deal with an attack. Yet you still don’t have a good handle on your disorder—the treatments aren’t helping as much as you need them too, and you’re rapidly losing the small amount of control you have. If this sounds like you, it might be a good idea to do some research about new migraine surgeries.
What is Migraine Surgery?
The goal of migraine surgery is to reduce or eliminate headache frequency, duration and pain. Migraines can be associated with compression and irritation of sensory nerves and vessels around your head. When these compression points are released during surgery, the severity of migraines may decrease or you may not experience further migraines.
Migraine surgery is a relatively new and evolving treatment option for individuals who suffer from chronic migraines that are unresponsive to other treatments. The procedure involves identifying and decompressing specific nerves or trigger points that may be contributing to the migraines. While some patients have reported significant improvement in their migraine symptoms after surgery, it’s important to note that this approach may not be suitable for everyone, and it comes with its own set of advantages and disadvantages:
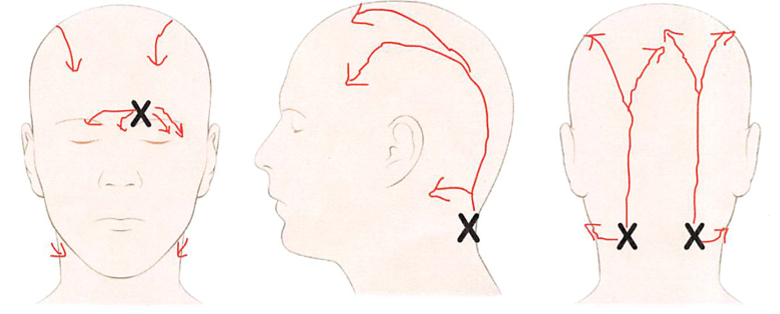
Sites of nerve compression are also known as trigger points. You may have one or several trigger points depending on your symptoms. The most common and main trigger sites are frontal (pain above your eyes and/or your forehead), temporal (pain over your temples), rhinogenic (pain inside your nose that can extend to behind your eyes), occipital (pain on the back of your head that can radiate across your skull to your eyes or behind your eyes). You may also experience pain at less common sites around your head.
What Are the good Aspects or bad Aspects of Migraine Surgeries ?
Advantages of Migraine Surgery:
- Reduction in Migraine Frequency and Severity: Some patients experience a significant reduction in the frequency, duration, and severity of their migraine attacks after surgery. This can lead to an improved quality of life for those who have been suffering from chronic migraines.
- Non-Drug Approach: Migraine surgery offers an alternative to medication-based treatments. For individuals who cannot tolerate or do not respond well to medications, surgery may be a viable option.
- Long-Lasting Relief: For those who respond positively to surgery, the benefits can be long-lasting. Some patients experience relief from migraines for several years or even permanently.
- Improved Quality of Life: Chronic migraines can be debilitating, impacting a person’s ability to work, socialize, and enjoy life. Successful migraine surgery can significantly enhance a patient’s overall quality of life.
Disadvantages of Migraine Surgery:
- Limited Effectiveness: Migraine surgery is not guaranteed to work for everyone. Success rates vary, and not all patients experience significant relief from their migraines. It may be challenging to predict who will benefit from the procedure.
- Surgical Risks: Like any surgery, migraine surgery carries inherent risks, such as infection, scarring, and anesthesia-related complications. Patients should carefully weigh the potential benefits against these risks.
- Cost: Migraine surgery can be expensive, and it may not be covered by insurance. The financial burden of the procedure can be a significant drawback for some patients.
- Recovery Time: Recovery from migraine surgery can take several weeks, during which time patients may experience discomfort and limited mobility. This can disrupt daily activities and work commitments.
- Possible Side Effects: Some patients may experience temporary or permanent side effects from the surgery, such as numbness, tingling, or weakness in the surgical area.
- Not a Cure-All: Migraine surgery is not a cure for all types of migraines. It primarily targets specific nerve compression issues, so it may not address the underlying causes of migraines in all patients.
- Lack of Long-Term Data: While there have been promising results reported in the short term, there is limited long-term data available on the outcomes of migraine surgery. It’s essential to consider the potential for migraine recurrence over time.
What is the Surgery Success Rate?
Most studies have shown success rates above 70 percent, with roughly one-third of the patients experiencing total relief of their migraines. When successful, patients report an improvement in migraine frequency, duration, intensity and in health-related quality-of-life.
Who is a Candidate for Migraine Surgery?
- Patients who have been diagnosed with migraines by a neurologist (not all headaches are migraines)
- Patients with sites of nerve compression identifiable with a high degree of confidence
Several other factors are considered, including the efficacy (or failure) of medical treatment, side effects of medications and the severity of the migraines. Patients with a favorable response to Botox® or local anesthetic injections are generally good candidates for migraine surgery.
Will I experience side effects or have scars?
Most complications are minor and temporary, and will vary according to the specific surgery. Treatment of migraines around the eye might actually improve the appearance of the forehead by decreasing wrinkles and correcting sagging eyebrows. Complications include wound healing problems, nerve injuries, bleeding and failure of surgery to ameliorate the headaches.
Most of the incisions are well hidden, either in the scalp or in the upper eyelid.
How long is the recovery?
Slight bruising and swelling may occur, and typically resolves within two weeks. Most patients are able to return to their usual activities in the same time frame. Depending on the specific nerves targeted by surgery, patients might be asked to avoid strenuous exercise for up to three weeks.
What Surgical Techniques Are Used to Treat Migraine ?
Migraine surgery typically involves the identification and decompression of specific nerves or trigger points that may be contributing to migraine attacks. Several surgical techniques have been developed to address different potential sources of migraines. It’s important to note that not all of these techniques are widely accepted or recommended, and the effectiveness of each may vary from person to person. Here are some surgical techniques that have been used to treat migraines:
- Frontal (Supraorbital) Migraine Surgery: This procedure targets the supraorbital nerve, which is located in the forehead. Surgeons make small incisions in the scalp and release or decompress this nerve to reduce migraine symptoms, particularly those associated with the forehead and eye area.
- Temporal (Temporalis) Migraine Surgery: Temporal migraine surgery focuses on the zygomaticotemporal branch of the trigeminal nerve, which is located in the temple area. Surgeons access this nerve through small incisions in the temples to relieve migraine symptoms in the temporal region.
- Occipital Migraine Surgery: Occipital migraine surgery aims to address the greater occipital nerve, which is located at the base of the skull. Surgeons decompress or release this nerve to reduce migraines that are concentrated in the back of the head and upper neck.
- Rhinogenic Migraine Surgery: Some surgeons believe that migraines can be triggered by nasal or sinus issues. Rhinogenic migraine surgery involves correcting structural problems in the nasal passages or sinuses to alleviate migraine symptoms.
- Trigger Point Deactivation: This approach involves identifying trigger points, such as muscle knots or areas of muscle tension, and releasing or deactivating these points through various surgical or minimally invasive techniques.
- Peripheral Nerve Decompression: In some cases, surgeons may explore the possibility of decompressing other peripheral nerves in the head and neck region that could be contributing to migraines. This approach is less standardized and may involve multiple nerve sites.
- Neurostimulation Devices: While not a traditional surgery, some individuals with chronic migraines may opt for implantable neurostimulation devices, such as occipital nerve stimulators or supraorbital nerve stimulators. These devices deliver electrical impulses to targeted nerves to help reduce migraine frequency and intensity.
It’s crucial to consult with a headache specialist or a surgeon who specializes in migraine surgery to determine which specific surgical technique, if any, is appropriate for your unique case. Migraine surgery is typically considered as a last resort for individuals with chronic migraines that have not responded well to other treatments, and the decision to undergo surgery should be made carefully after a thorough evaluation of potential risks and benefits. Additionally, the availability of these surgical techniques may vary by region and healthcare provider expertise.
Cautions From Headache Specialists
Despite reported successes, many neurologists and headache specialists are reluctant to embrace these surgeries as part of the standard treatment for migraines. They want to see more study. And, the US Food and Drug Administration has not approved the procedures for migraine relief.
Richard Kim, MD, neurologist and headache specialist, Premier Health Clinical Neuroscience Institute, thinks that cutting or decompressing a nerve to “cure” migraines is too simplistic.
“Migraine is a genetic disorder. It’s not just a peripheral mechanism. The headache community thinks there’s not enough good data to know if these headache procedures are really effective or not.”
He cites an article on the Choosing Wisely website of the American Board of Internal Medicine Foundation (ABIM). In the 2013 article, the American Headache Society advises physicians: “Don’t recommend surgical deactivation of migraine trigger points outside of a clinical trial.”
Both Dr. Kim and the Headache Society are concerned that current evidence is based on small controlled trials and observation. They advocate for large multicenter, randomized, controlled trials with long-term follow-up to provide more definitive proof that these surgeries will have lasting benefit and not cause harmful side effects.
“The surgery may work, but good, quality, evidence-based research is not there. A lot of the studies on these procedures have been criticized for not carefully defining which patients would be appropriate for this. We also don’t know if patients continued with preventive medications, which would affect the results.”
Side Effects and Potential Complications of Migraine Surgery
Migraine surgery, like any surgical procedure, can have side effects and potential complications. It’s essential for individuals considering this treatment option to be aware of these risks and discuss them thoroughly with their healthcare provider. The specific side effects and complications can vary depending on the type of migraine surgery and individual factors, but here are some potential side effects and risks associated with migraine surgery:
- Pain and Discomfort: After migraine surgery, it is common to experience pain, swelling, and discomfort at the surgical site. This discomfort may persist for several days or weeks, depending on the surgical approach.
- Numbness and Tingling: Nerve decompression procedures can lead to temporary or, in some cases, permanent numbness or tingling in the areas affected by the surgery. This can include the forehead, temple, or back of the head, depending on the specific surgery performed.
- Scarring: Surgical incisions can result in visible scars. The size and appearance of scars can vary depending on the surgical technique and individual healing factors.
- Infection: Any surgical procedure carries a risk of infection at the incision site. Proper wound care and hygiene are essential to minimize this risk.
- Bleeding: Surgical procedures can lead to bleeding, both during the operation and in the post-operative period. Excessive bleeding may require additional medical attention.
- Anesthesia Risks: General anesthesia or local anesthesia used during the surgery carries its own set of risks, including allergic reactions, breathing difficulties, and anesthesia-related complications.
- Unsatisfactory Outcomes: There is no guarantee that migraine surgery will provide significant relief from migraine symptoms. Some individuals may not experience the expected benefits, and their migraines may persist.
- Recurrence of Migraines: Even if the surgery initially reduces migraine frequency and severity, migraines can sometimes recur over time.
- Additional Surgeries: In some cases, individuals may require additional surgeries or procedures if the initial surgery does not provide the desired results or if complications arise.
- Long-Term Effects: The long-term effects of migraine surgery are still being studied, and there may be unforeseen consequences that become apparent over time.
Pain Medications, Pain Relief, and Pain Management