Menopausal hot flashes are sudden, intense feelings of heat that are commonly experienced by women during the menopausal transition, typically in their late 40s or early 50s. Hot flashes can cause a flushed face, sweating, and a rapid heartbeat, and they are often followed by a feeling of cold or clammy skin.
The underlying cause of hot flashes during menopause is hormonal changes, specifically a decline in estrogen levels. Estrogen plays a role in regulating body temperature, and as its levels decrease during menopause, the body’s temperature regulation can become more sensitive, leading to hot flashes.

Treatment options for menopausal hot flashes include:
- Hormone Replacement Therapy (HRT): This involves taking estrogen or a combination of estrogen and progestin to replace the hormones that decline during menopause. HRT can effectively reduce hot flashes, but it is not suitable for everyone and may have associated risks.
- Non-hormonal Medications: Certain medications, such as selective serotonin reuptake inhibitors (SSRIs), selective norepinephrine reuptake inhibitors (SNRIs), and gabapentin, have been found to be effective in reducing the frequency and severity of hot flashes.
- Lifestyle Modifications: Making certain lifestyle changes can also help manage hot flashes. These include maintaining a healthy weight, practicing relaxation techniques such as deep breathing or yoga, avoiding triggers like spicy foods and caffeine, and dressing in layers to manage body temperature.
- Herbal Remedies: Some women find relief from hot flashes with herbal supplements such as black cohosh or soy isoflavones. However, the effectiveness of these remedies can vary, and it’s essential to discuss their use with a healthcare provider.
Medical treatments for menopausal hot flashes include the following options:
- Hormone Replacement Therapy (HRT): This is a common medical treatment that involves providing the body with the estrogen it lacks to alleviate symptoms such as hot flashes during menopause. HRT typically includes a combination of estrogen and progestin. However, HRT needs to be assessed based on individual health conditions, and it may be associated with certain health risks.
- Selective Estrogen Receptor Modulators (SERMs): SERMs are a class of drugs that mimic the action of estrogen and can be used to alleviate menopausal symptoms, including hot flashes, without affecting breast and uterine tissues in the same way as estrogen. Raloxifene is an example of a SERM.
- Antidepressant Medications: Some antidepressants, such as paroxetine and venlafaxine, have been found to have a certain effect in relieving hot flashes. The use of these medications should be supervised by a doctor.
- Antiepileptic Drugs: Certain antiepileptic drugs, such as gabapentin and pregabalin, are also used to treat symptoms of hot flashes. They work by affecting the nervous system to alleviate symptoms.

Extended-release (ER) gabapentin (Serada, Depomed), an investigational nonhormonal drug, improves sleep and reduces hot flashes in menopausal women, according to a phase 3 clinical trial known as BREEZE 3.
The results were presented here at the North American Menopause Society (NAMS) 23rd Annual Meeting.
“Right now, if women don’t want to take hormones, and if over-the-counter products, acupuncture, and lifestyle changes do not work, we don’t have any FDA [US Food and Drug Administration] approved therapies,” said lead researcher JoAnn Pinkerton, MD, who is professor of obstetrics and gynecology at the University of Virginia in Charlottesville and past president of NAMS.
A New Drug Application was submitted for gabapentin ER in July. If approved, the drug will be the first nonhormonal, nonantidepressant treatment for the bothersome symptoms of menopause, Dr. Pinkerton explained.
BREEZE 3 looked at the effect of gabapentin ER on hot flashes and on sleep. Data were presented in 2 different abstracts by 2 different investigators.
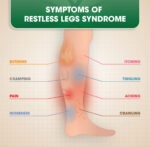
Gabapentin is used to control epileptic seizures and restless leg syndrome, and recently was approved by the FDA for the treatment of postherpetic neuralgia.
The ER formulation was developed to be taken twice a day instead of 3 times a day, which significantly decreases the adverse-effect profile, Dr. Pinkerton said.
“With the short-acting version, 20% of patients were somnolent or dizzy. In this trial, with the extended-release formulation, the rate of somnolence or dizziness started at 11% and went down to 3% very quickly. It was very well tolerated and very few people discontinued treatment because of those symptoms,” she said. At the end of 6 months, people felt significantly better, she added.
Gabapentin Improves Insomnia
In the sleep part of BREEZE 3, gabapentin was found to have a positive impact on sleep disturbance. Researchers assessed the impact of gabapentin using 2 measures of sleep: the Insomnia Severity Index (ISI) score and the daily sleep interference (S/I) score.
At baseline, the mean ISI scores were 17.54 in the gabapentin group and 17.33 in the placebo group, indicating moderate insomnia, and the mean S/I scores were 7.3 and 7.4, respectively, indicating a moderate to severe sleep disturbance.
After 12 weeks, there was a clinically meaningful reduction in ISI score in the gabapentin group, compared with the placebo group (8.7 vs 6.3; P = .0044), and in S/I score (3.6 vs 2.8;P = .0056). Reductions out to week 24 were maintained in the ISI score (8.6 vs 6.2; P = .0068) and in the S/I score (3.9 vs 3.0; P = .0084).
“I was happy that sleep was looked at in an objective way. If you ask many women, their hot flushes at night really bother them. If they can’t sleep because of hot flushes, they basically cannot function during the day, so we need to look at sleep separately,” said Risa Kagan, MD, from East Bay Physicians Medical Group, Alta Bates Summit Medical Center, in Berkeley, and clinical professor in the Department of Obstetrics, Gynecology, and Reproductive Sciences at the University of California, San Francisco, who led the sleep part of BREEZE 3.
Dr. Kagan added that, although it is fine to look at all of the data objectively, in the end, the aim is to help women transition through the menopause. “This was not just a placebo effect, this was actually a statistically significant improvement in sleep over placebo,” she explained.
http://www.medscape.com/viewarticle/772249
What is Hot Flash ?
A hot flash is the sudden feeling of warmth in the upper body, which is usually most intense over the face, neck and chest. Your skin might redden, as if you’re blushing. A hot flash can also cause sweating. If you lose too much body heat, you might feel chilled afterward. Night sweats are hot flashes that happen at night, and they may disrupt your sleep.
Although other medical conditions can cause them, hot flashes most commonly are due to menopause — the time when menstrual periods become irregular and eventually stop. In fact, hot flashes are the most common symptom of the menopausal transition.
There are a variety of treatments for bothersome hot flashes.

Symptoms of Hot Flash
During a hot flash, you might have:
- A sudden feeling of warmth spreading through your chest, neck and face
- A flushed appearance with red, blotchy skin
- Rapid heartbeat
- Perspiration, mostly on your upper body
- A chilled feeling as the hot flash lets up
- Feelings of anxiety
The frequency and intensity of hot flashes vary among women. Hot flashes may be mild or so intense that they disrupt daily activities. They can happen at any time of day or night. Nighttime hot flashes (night sweats) may wake you from sleep and can cause long-term sleep disruptions.
How often hot flashes occur varies among women, but most women who report having hot flashes experience them daily. On average, hot flash symptoms persist for more than seven years. Some women have them for more than 10 years.
Hot Flash Diagnosis
Your doctor can usually diagnose hot flashes based on a description of your symptoms. Your doctor might suggest blood tests to check whether you’re in menopausal transition.
Hot Flash Treatment
The most effective way to relieve the discomfort of hot flashes is to take estrogen, but taking this hormone carries risks. If estrogen is appropriate for you and you start it within 10 years of your last menstrual period or before age 60, the benefits can be greater than the risks.
Medications such as antidepressants and anti-seizure drugs also might help reduce hot flashes, although they’re less effective than hormones.
Discuss the pros and cons of various treatments with your doctor. If hot flashes don’t interfere with your life, you probably don’t need treatment. Hot flashes subside gradually for most women, even without treatment, but it can take several years for them to stop.
Hormone therapy
Estrogen is the primary hormone used to reduce hot flashes. Most women who have had a hysterectomy can take estrogen alone. But if you still have a uterus, you should take progesterone with estrogen to protect against cancer of the lining of the uterus (endometrial cancer).
With either regimen, the therapy needs to be tailored to your needs. Guidelines suggest using the smallest effective dose for symptom control. How long you use the treatment depends on the balance of your risks and benefits from hormone therapy. The goal is to optimize your quality of life.
Some women who take progesterone with estrogen therapy experience progesterone-related side effects. For women who can’t tolerate oral progesterone, a combination drug of bazedoxifene with conjugated estrogens (Duavee) is also approved for treating menopausal symptoms. Like progesterone, taking bazedoxifene with estrogen may help you avoid the increased risk of endometrial cancer from estrogen alone. Bazedoxifene might also protect your bones.
If you have had or are at risk of breast or endometrial cancer, heart disease, stroke or blood clots, talk to your doctor about whether estrogen therapy is right for you.
Antidepressants
A low-dose form of paroxetine (Brisdelle) is the only nonhormone treatment for hot flashes approved by the U.S. Food and Drug Administration. Other antidepressants that have been used to treat hot flashes include:
- Venlafaxine (Effexor XR)
- Paroxetine (Paxil, Pexeva)
- Citalopram (Celexa)
- Escitalopram (Lexapro)
These medications aren’t as effective as hormone therapy for severe hot flashes, but they can be helpful to women who can’t use hormones. Possible side effects include nausea, difficulty sleeping or drowsiness, weight gain, dry mouth or sexual dysfunction.
Other prescription medications
Other medications that might offer relief for some women include:
- Gabapentin (Neurontin, Gralise, others). Gabapentin is an anti-seizure medication that’s moderately effective in reducing hot flashes. Side effects can include drowsiness, dizziness, water retention in the limbs (edema) and fatigue.
- Pregabalin (Lyrica). Pregabalin is another anti-seizure medication that can be effective in reducing hot flashes. Side effects can include dizziness, drowsiness, difficulty concentrating and weight gain.
- Oxybutynin (Ditropan XL, Oxytrol). Oxybutynin is a pill or patch most often used to treat urinary conditions like overactive bladder. It may also help relieve hot flashes in some women. Side effects can include dry mouth, dry eyes, constipation, nausea and dizziness.
- Clonidine (Catapres, Kapvay, others). Clonidine, a pill or patch typically used to treat high blood pressure, might provide some relief from hot flashes. Side effects include dizziness, drowsiness, dry mouth and constipation.
Nerve block procedure
A procedure known as stellate ganglian block has shown promise for treating moderate to severe hot flashes, but more research is needed. It involves injecting an anesthetic into a nerve cluster in the neck. The treatment has been used for pain management. Side effects include pain and bruising at the injection site.
Pain Medications, Pain Relief, and Pain Management