Anemia is a medical condition characterized by a decrease in the number of red blood cells (RBCs) or a decrease in the amount of hemoglobin in the blood. Hemoglobin is a protein present in red blood cells that binds to oxygen and carries it to tissues and organs throughout the body. Anemia leads to a reduced capacity of the blood to carry oxygen to various parts of the body, resulting in symptoms such as fatigue, weakness, and paleness.
Anemia is defined as a low number of red blood cells. In a routine blood test, anemia is reported as a low hemoglobin or hematocrit. Hemoglobin is the main protein in your red blood cells. It carries oxygen and delivers it throughout your body. If you have anemia, your hemoglobin level will be low, too. If it is low enough, your tissues or organs may not get enough oxygen. Symptoms of anemia – like fatigue or shortness of breath – happen because your organs aren’t getting what they need to work the way they should.
Anemia is the most common blood condition in the U.S. It affects almost 6% of the population. Women, young children, and people with long-term diseases are more likely to have anemia. Important things to remember are:
- Certain forms of anemia are passed down through your genes, and infants may have it from birth.
- Women are at risk of iron-deficiency anemia because of blood loss from their periods and higher blood supply demands during pregnancy.
- Older adults have a greater risk of anemia because they are more likely to have kidney disease or other chronic medical conditions.
There are several types of anemia, and each type has different causes and treatments. The four main causes of anemia include:
- Blood Loss: Anemia can occur when there is a significant loss of blood due to conditions such as heavy menstrual periods, gastrointestinal bleeding (ulcers, tumors, or colorectal cancer), or trauma.
- Decreased or Faulty Red Blood Cell Production: This can be caused by nutritional deficiencies (such as iron, vitamin B12, or folic acid), bone marrow disorders, chronic diseases (such as chronic kidney disease), or inherited conditions (like sickle cell anemia or thalassemia).
- Destruction of Red Blood Cells: Some medical conditions can lead to the destruction of red blood cells at an accelerated rate. This can be due to inherited conditions (like hemolytic anemias) or acquired conditions (such as autoimmune disorders).
- Vitamin B12-deficiency Anemia: Vitamin B12–deficiency anemia, also known as cobalamin deficiency, is a condition that develops when your body can’t make enough healthy red blood cells because it doesn’t have enough vitamin B12. Your body needs vitamin B12 to make healthy , , and . Since your body doesn’t make vitamin B12, you have to get it from the foods you eat or from supplements.
Mild anemia is a common and treatable condition that can develop in anyone. It may come about suddenly or over time, and may be caused by your diet, medicines you take, or another medical condition. Anemia can also be chronic, meaning it lasts a long time and may never go away completely. Some types of anemia are inherited. The most common type of anemia is iron-deficiency anemia.
Some people are at a higher risk for anemia, including women during their menstrual periods and pregnancy. People who do not get enough iron or certain vitamins and people who take certain medicines or treatments are also at a higher risk.
Anemia may also be a sign of a more serious condition, such as bleeding in your stomach, inflammation from an infection, kidney disease, cancer, or autoimmune diseases. Your doctor will use your medical history, a physical exam, and test results to diagnose anemia.
Treatments for anemia depend on the type you have and how serious it is. For some types of mild to moderate anemia, you may need iron supplements, vitamins, or medicines that make your body produce more red blood cells. To prevent anemia in the future, your doctor may also suggest healthy eating changes.
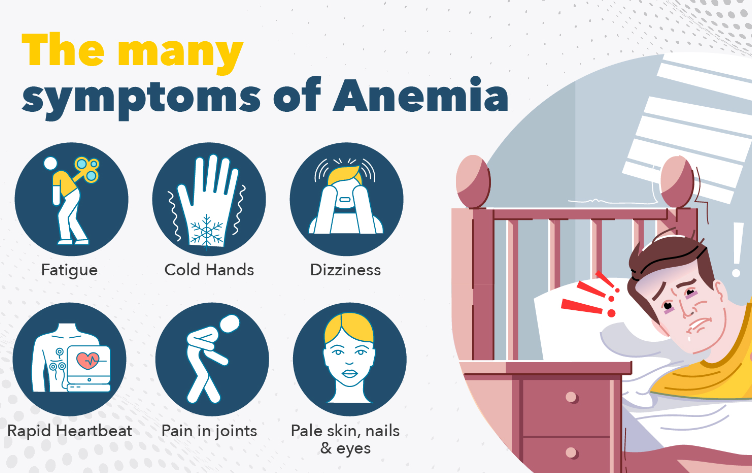
The Symptoms of Anemia
The symptoms of anemia can vary depending on the underlying cause, the severity of the condition, and individual differences. Anemia symptoms depend on the cause and how bad the anemia is. Anemia can be so mild that it causes no symptoms at first. But symptoms usually then occur and get worse as the anemia gets worse.
If another disease causes the anemia, the disease can mask the anemia symptoms. Then a test for another condition might find the anemia. Certain types of anemia have symptoms that point to the cause.
Common symptoms of anemia include:
- Fatigue and Weakness: A common and often early symptom of anemia is a feeling of tiredness or weakness, even with normal activities. This occurs because the body’s tissues and organs aren’t getting enough oxygen.
- Pale or Sallow Skin: Anemia can cause a reduction in the number of red blood cells, leading to paleness or a sallow complexion.
- Shortness of Breath: Inadequate oxygen delivery to tissues can result in shortness of breath, especially during physical activities.
- Dizziness or Lightheadedness: Reduced oxygen levels in the blood can affect the brain, leading to feelings of dizziness or lightheadedness.
- Cold Hands and Feet: Poor circulation of oxygenated blood may cause extremities to feel cold.
- Headache: Anemia can sometimes lead to headaches, especially when the brain doesn’t receive enough oxygen.
- Irritability: Reduced oxygen levels in the body can affect mood and lead to irritability.
- Irregular Heartbeats (Arrhythmias): In severe cases, anemia can lead to irregular heartbeats or an enlarged heart as the heart tries to compensate for the reduced oxygen-carrying capacity of the blood.
- Brittle Nails and Hair Loss: In some cases, anemia may affect the health of nails and hair.
- Chest pain
- Irregular heartbeat
- Difficulty Concentrating: Inadequate oxygen supply to the brain can result in difficulty concentrating and problems with memory.
The Causes of Anemia
Anemia can have various causes, and it is essential to identify the specific underlying factor to determine the most appropriate treatment.
Different types of anemia have different causes. They include:
- Iron deficiency anemia. Too little iron in the body causes this most common type of anemia. Bone marrow needs iron to make hemoglobin. Without enough iron, the body can’t make enough hemoglobin for red blood cells. Pregnant people can get this type of anemia if they don’t take iron supplements. Blood loss also can cause it. Blood loss might be from heavy menstrual bleeding, an ulcer, cancer or regular use of some pain relievers, especially aspirin.
- Vitamin deficiency anemia. Besides iron, the body needs folate and vitamin B-12 to make enough healthy red blood cells. A diet that doesn’t have enough of these and other key nutrients can result in the body not making enough red blood cells. Also, some people can’t absorb vitamin B-12. This can lead to vitamin deficiency anemia, also called pernicious anemia.
- Anemia of inflammation. Diseases that cause ongoing inflammation can keep the body from making enough red blood cells. Examples are cancer, HIV/AIDS, rheumatoid arthritis, kidney disease and Crohn’s disease.
- Aplastic anemia. This rare, life-threatening anemia occurs when the body doesn’t make enough new blood cells. Causes of aplastic anemia include infections, certain medicines, autoimmune diseases and being in contact with toxic chemicals.
- Anemias linked to bone marrow disease. Diseases such as leukemia and myelofibrosis can affect how the bone marrow makes blood. The effects of these types of diseases range from mild to life-threatening.
- Hemolytic anemias. This group of anemias is from red blood cells being destroyed faster than bone marrow can replace them. Certain blood diseases increase how fast red blood cells are destroyed. Some types of hemolytic anemia can be passed through families, which is called inherited.
- Sickle cell anemia. This inherited and sometimes serious condition is a type of hemolytic anemia. An unusual hemoglobin forces red blood cells into an unusual crescent shape, called a sickle. These irregular blood cells die too soon. That causes an ongoing shortage of red blood cells.
The causes of anemia can be broadly categorized into three main groups:
- Blood Loss:
- Menstrual Blood Loss: In women of childbearing age, heavy or prolonged menstrual periods can lead to significant blood loss, resulting in iron-deficiency anemia.
- Gastrointestinal Bleeding: Conditions such as ulcers, gastritis, colorectal cancer, or gastrointestinal lesions can cause chronic bleeding and lead to anemia.
- Trauma or Surgery: Severe injuries or surgical procedures that result in substantial blood loss can lead to acute anemia.
- Decreased or Faulty Red Blood Cell Production:
- Nutritional Deficiencies: Inadequate intake of essential nutrients such as iron, vitamin B12, or folic acid can impair the body’s ability to produce red blood cells.
- Bone Marrow Disorders: Diseases affecting the bone marrow, where red blood cells are produced, can lead to reduced red blood cell production. Examples include aplastic anemia or myelodysplastic syndromes.
- Chronic Diseases: Certain chronic conditions, such as chronic kidney disease or inflammatory disorders, can interfere with red blood cell production.
- Destruction of Red Blood Cells (Hemolysis):
- Inherited Conditions: Conditions like sickle cell anemia, thalassemia, and hereditary spherocytosis can lead to the premature destruction of red blood cells.
- Autoimmune Disorders: Conditions where the immune system mistakenly attacks and destroys red blood cells, such as autoimmune hemolytic anemia.
- Infections: Certain infections, such as malaria or some bacterial or viral infections, can lead to the destruction of red blood cells.
It’s important to note that anemia can be a symptom of an underlying health issue rather than a standalone condition. Additionally, some individuals may have a combination of factors contributing to their anemia.
Diagnosing the specific cause of anemia typically involves a thorough medical history, physical examination, and blood tests, including a complete blood count (CBC) and additional tests to measure iron levels, vitamin B12, and folic acid. Treatment will depend on addressing the underlying cause and may include dietary changes, supplements, medications, or other interventions as necessary.
How Serious is Anemia?
The seriousness of anemia depends on various factors, including the underlying cause, the severity of the condition, and how quickly it develops. In general, mild cases of anemia may cause minimal symptoms or discomfort, while more severe cases can lead to significant health complications. Here are some considerations regarding the seriousness of anemia:
- Mild Anemia:
- Mild forms of anemia may not cause noticeable symptoms or may result in only mild fatigue or weakness.
- In some cases, individuals with mild anemia may be asymptomatic and may not be aware of their condition without a blood test.
- While mild anemia may not pose an immediate threat, addressing the underlying cause and correcting the anemia is essential to prevent its progression.
- Moderate Anemia:
- Moderate anemia is characterized by a more significant decrease in red blood cell count or hemoglobin levels.
- Symptoms such as fatigue, weakness, paleness, shortness of breath, and dizziness may become more pronounced.
- Individuals with moderate anemia may experience a decreased ability to perform daily activities and may feel increasingly fatigued.
- Severe Anemia:
- Severe anemia is a serious medical condition that requires prompt attention and intervention.
- Symptoms become more severe, and individuals may experience extreme fatigue, rapid heart rate, difficulty concentrating, headache, and chest pain.
- Severe anemia can lead to complications such as heart failure, especially in individuals with pre-existing cardiovascular conditions.
- In acute cases, severe anemia may require emergency medical attention and blood transfusions.
- Impact on Specific Groups:
- Anemia can be particularly concerning for certain populations, such as pregnant women and young children. In these groups, anemia can affect the health of both the mother and the developing fetus or child.
- Chronic Anemia:
- Long-term or chronic anemia, if left untreated, can contribute to fatigue, weakness, and a reduced quality of life.
- Chronic anemia may also exacerbate underlying health conditions and increase the risk of complications, especially in individuals with chronic diseases.
The Risk Factors of Anemia
Several risk factors increase the likelihood of developing anemia. Understanding these risk factors can help individuals and healthcare professionals identify those who may be more susceptible to the condition. Common risk factors for anemia include:
- Nutritional Deficiencies:
- Iron Deficiency: Inadequate dietary intake of iron, especially in populations with poor nutrition, vegetarian diets, or conditions that impair iron absorption.
- Vitamin B12 Deficiency: Poor dietary intake of vitamin B12 (commonly found in animal products), pernicious anemia (a condition where the body can’t absorb enough B12), or certain gastrointestinal disorders affecting B12 absorption.
- Age and Gender:
- Children and Adolescents: Rapid growth during childhood and adolescence may increase the demand for nutrients, making these age groups more susceptible to nutritional deficiencies.
- Women of Childbearing Age: Menstrual blood loss, especially in women with heavy or prolonged periods, increases the risk of iron-deficiency anemia.
- Medical Conditions:
- Chronic Diseases: Conditions such as chronic kidney disease, inflammatory disorders (rheumatoid arthritis, inflammatory bowel disease), and chronic infections can contribute to anemia.
- Autoimmune Disorders: Conditions like lupus, rheumatoid arthritis, and other autoimmune disorders can lead to hemolytic anemia, where the immune system attacks and destroys red blood cells.
- Cancer: Certain cancers, especially those affecting the gastrointestinal tract or bone marrow, can lead to anemia.
- Genetic Factors:
- Inherited Anemias: Conditions like sickle cell anemia, thalassemia, and hereditary spherocytosis are inherited disorders that increase the risk of anemia.
- Gastrointestinal Disorders:
- Malabsorption: Disorders such as celiac disease or inflammatory bowel disease can lead to nutrient malabsorption, including iron and vitamin B12.
- Gastrointestinal Bleeding: Ulcers, tumors, or lesions in the gastrointestinal tract can result in chronic bleeding, leading to anemia.
- Pregnancy:
- Increased Blood Volume: The expansion of blood volume during pregnancy, coupled with the growing demands of the developing fetus, can lead to iron deficiency anemia if maternal iron stores are insufficient.
- Chronic Medication Use:
- Certain Medications: Prolonged use of medications like nonsteroidal anti-inflammatory drugs (NSAIDs), anticoagulants, or medications that interfere with nutrient absorption can contribute to anemia.
- Race and Ethnicity:
- Certain Populations: People of African, Asian, or Mediterranean descent may have a higher risk of specific inherited anemias, such as sickle cell anemia or thalassemia.
Anemia Diagnosis
A complete blood count (CBC) test will measure your red blood cells, hemoglobin, and other parts of your blood. Your doctor will ask about your family history and your medical history after the CBC. They’ll probably do some tests, including:
- Blood smear or differential to count your white blood cells, check the shape of your red blood cells, and look for unusual cells
- Reticulocyte count to check for immature red blood cells
The Treatment of Anemia
The treatment of anemia depends on the underlying cause and severity of the condition. The primary goal is to address the root cause of the anemia and, when necessary, to replenish or enhance the production of red blood cells. Here are common approaches to anemia treatment:
- Iron Supplementation:
- For iron-deficiency anemia, which is one of the most common types, iron supplements are often prescribed. These may include oral iron supplements or, in severe cases or when oral supplementation is not effective, intravenous iron.
- Vitamin and Nutrient Supplements:
- If anemia is due to deficiencies in vitamin B12, folic acid, or other nutrients, supplementation with these vitamins may be recommended.
- Dietary Changes:
- Increasing the intake of iron-rich foods, such as red meat, poultry, fish, beans, lentils, fortified cereals, and leafy green vegetables, can help address iron-deficiency anemia.
- Treatment of Underlying Conditions:
- If anemia is a result of an underlying medical condition, such as chronic kidney disease, inflammatory disorders, or gastrointestinal bleeding, treating the primary condition is crucial. This may involve medications, lifestyle changes, or other interventions.
- Erythropoiesis-Stimulating Agents (ESAs):
- In certain cases, especially in chronic kidney disease or cancer-related anemia, medications known as ESAs may be prescribed to stimulate the production of red blood cells.
- Blood Transfusion:
- In cases of severe anemia or acute blood loss, a blood transfusion may be necessary to quickly increase the number of red blood cells and improve oxygen-carrying capacity.
- Bone Marrow Stimulants:
- For some types of anemia, such as aplastic anemia, medications that stimulate bone marrow function may be used to increase red blood cell production.
- Treatment during Pregnancy:
- Pregnant women with anemia may require iron supplementation and careful monitoring to ensure both maternal and fetal well-being.
- Lifestyle Changes:
- Adopting a healthy lifestyle, including regular exercise and a balanced diet, can support overall health and contribute to the management of anemia.
It is crucial for individuals with anemia to work closely with healthcare professionals to determine the most appropriate treatment plan. Self-diagnosis and self-treatment can be ineffective and may lead to complications. Regular follow-up visits and monitoring of blood levels are typically necessary to assess the response to treatment and adjust the plan if needed. In some cases, ongoing management may be required to prevent recurrence of anemia.
The Prevention of Anemia
Preventing anemia involves addressing the underlying causes and adopting lifestyle practices that support optimal blood health. Here are several strategies for preventing anemia:
- Maintain a Nutrient-Rich Diet:
- Consume a balanced diet that includes a variety of foods rich in essential nutrients such as iron, vitamin B12, folic acid, and vitamin C.
- Iron-rich foods include red meat, poultry, fish, beans, lentils, fortified cereals, and leafy green vegetables.
- Foods high in vitamin B12 include meat, fish, eggs, and dairy products.
- Folic acid is found in leafy greens, citrus fruits, fortified cereals, and legumes.
- Anemia dietTo treat anemia, eat an iron-rich diet. If you don’t eat enough iron, your body can become iron-deficient. Some foods that have high amounts of iron include:
- Meats
- Eggs
- Leafy green veggies
- Iron-fortified foods like cereals
- Beans
- Seafood
- Peas
- Nuts and dried fruit
- Lentils
- Supplementation:
- If there is a risk of nutritional deficiencies, consider taking dietary supplements under the guidance of a healthcare professional. This is especially relevant for individuals with dietary restrictions, such as vegetarians or vegans.
- Iron Absorption Enhancers:
- Consume foods that enhance iron absorption when consuming plant-based iron sources. Vitamin C-rich foods, such as citrus fruits and tomatoes, can enhance the absorption of non-heme iron found in plant foods.
- Limit Iron Absorption Inhibitors:
- Avoid consuming substances that can inhibit iron absorption when consuming iron-rich foods. These include tea, coffee, and calcium supplements taken with meals.
- Prenatal Care:
- Pregnant women should receive regular prenatal care, including iron supplementation if necessary, to prevent iron-deficiency anemia, which is common during pregnancy.
- Manage Menstrual Health:
- Women with heavy or prolonged menstrual periods should seek medical advice and consider appropriate management strategies. This may include iron supplementation during menstruation.
- Regular Health Check-ups:
- Regularly monitor health and undergo routine blood tests, especially for individuals with chronic conditions or those at risk of specific types of anemia.
- Exercise Regularly:
- Regular physical activity supports overall health and can contribute to the maintenance of healthy blood levels. However, excessive exercise may contribute to iron loss, so balance is essential.
- Hydration:
- Stay adequately hydrated, as dehydration can affect blood volume and concentration.
- Avoid Smoking:
- Smoking can negatively impact blood circulation and oxygen delivery. Quitting smoking can contribute to overall cardiovascular health.
- Moderate Alcohol Consumption:
- Excessive alcohol intake can interfere with nutrient absorption and contribute to nutritional deficiencies. Moderation is key.
It’s important to note that preventing anemia may involve individualized strategies based on factors such as age, gender, health status, and lifestyle. If anemia is suspected or diagnosed, seeking guidance from a healthcare professional is crucial to determine the underlying cause and develop an appropriate prevention and treatment plan.
Anemia and Pregnancy
When you get pregnant, your body goes through many changes. Your body produces 20% to 30% more blood, which means you need more iron and vitamins.