What are anti-depressants?
Antidepressant medications are a first-choice option for treating major depressive disorder (MDD), according to guidelines from the American Psychiatric Association. They can also help to treat anxiety conditions, including generalized anxiety disorder.
There are various classes of antidepressant medications, each with different mechanisms of action. It’s important to note that the efficacy and side effects of these medications can vary among individuals, and the choice of antidepressant is often based on the specific characteristics of the patient and their condition. Here is a list of some common classes of antidepressants along with examples:
- Selective Serotonin Reuptake Inhibitors (SSRIs):
- Mechanism: Increase the levels of serotonin in the brain by inhibiting its reuptake.
- Examples:
- Fluoxetine (Prozac)
- Sertraline (Zoloft)
- Paroxetine (Paxil)
- Escitalopram (Lexapro)
- Citalopram (Celexa)
- Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs):
- Mechanism: Increase levels of both serotonin and norepinephrine.
- Examples:
- Venlafaxine (Effexor)
- Duloxetine (Cymbalta)
- Desvenlafaxine (Pristiq)
- Tricyclic Antidepressants (TCAs):
- Mechanism: Block the reuptake of serotonin and norepinephrine, but they also affect other receptors.
- Examples:
- Amitriptyline
- Imipramine
- Nortriptyline
- Monoamine Oxidase Inhibitors (MAOIs):
- Mechanism: Inhibit the activity of the enzyme monoamine oxidase, which breaks down neurotransmitters like serotonin, norepinephrine, and dopamine.
- Examples:
- Phenelzine (Nardil)
- Tranylcypromine (Parnate)
- Isocarboxazid (Marplan)
- Atypical Antidepressants:
- Mechanism: Various mechanisms of action; they don’t fit neatly into the above categories.
- Examples:
- Bupropion (Wellbutrin)
- Mirtazapine (Remeron)
- Trazodone (Desyrel)
- Norepinephrine-Dopamine Reuptake Inhibitors (NDRIs):
- Mechanism: Inhibit the reuptake of both norepinephrine and dopamine.
- Example:
- Bupropion (Wellbutrin)
There are different types of antidepressants, based on how they work within the brain. Some are better for treating certain conditions and symptoms. But they all come with potential side effects.
Generally, each type causes somewhat different side effects, but there can still be some variance within a single type.
People can also respond differently to antidepressants. Some people may have no troubling side effects, while others may have one or more serious side effects. This is why you may need to try a few different medications before you find the right fit.
Here’s a look at the main types of antidepressants and some of the side effects commonly associated with them. If you take a certain type, you probably won’t experience all of the side effects associated with it. You might also experience other side effects, including some serious ones, that aren’t listed here.
Some of the antidepressants used for pain relief are the older tricyclics. These come with numerous side effects classified as anticholinergic, including dry mouth, difficulty urinating, blurred vision, and constipation. Other possible side effects include lower blood pressure, fast heart beat, palpitations, weight gain, and fatigue.
A few of the newer antidepressants also reduce pain — and with less risk of anticholinergic issues. Still, the serotonin norepinephrine reuptake inhibitors (SNRIs) may cause the following common side effects:
- Anorexia
- Asthenia
- Constipation
- Dizziness
- Dry mouth
- Ejaculatory difficulties
- Headache
- Insomnia
- Nausea
- Nervousness
- Sweating
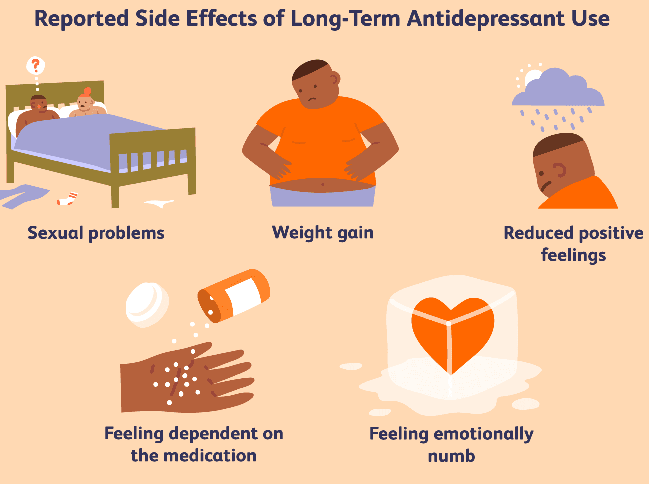
Anti-Depressant Side Effects
It’s important to continue treatment, even if you’re affected by side effects, as it will take several weeks before you begin to benefit from treatment. With time, you should find that the benefits of treatment outweigh any problems from side effects.
During the first few months of treatment, you’ll usually see your doctor or a specialist nurse at least once every 2 to 4 weeks to see how well the medicine is working.
For more information about your specific medicine, see the patient information leaflet that comes with it.
SSRIs and SNRIs
Common side effects of selective serotonin reuptake inhibitors (SSRIs) and serotonin-noradrenaline reuptake inhibitors (SNRIs) can include:
- feeling agitated, shaky or anxious
- feeling and being sick
- indigestion and stomach aches
- diarrhoea or constipation
- loss of appetite
- dizziness
- not sleeping well (insomnia), or feeling very sleepy
- headaches
- low sex drive
- difficulties achieving orgasm during sex or masturbation
- in men, difficulties obtaining or maintaining an erection (erectile dysfunction)
These side effects should improve within a few weeks, although some can occasionally persist.
Tricyclic antidepressants (TCAs)
Common side effects of TCAs can include:
- dry mouth
- slight blurring of vision
- constipation
- problems passing urine
- drowsiness
- dizziness
- weight gain
- excessive sweating (especially at night)
- heart rhythm problems, such as noticeable palpitations or a fast heartbeat (tachycardia)
The side effects should ease after a couple of weeks as your body begins to get used to the medicine.
Potential health risks
Serotonin syndrome
Serotonin syndrome is an uncommon, but potentially serious, set of side effects linked to SSRIs and SNRIs.
Serotonin syndrome occurs when the levels of a chemical called serotonin in your brain become too high. It’s usually triggered when you take an SSRI or SNRI in combination with another medicine (or substance) that also raises serotonin levels, such as another antidepressant or St John’s Wort.
Symptoms of serotonin syndrome can include:
- confusion
- agitation
- muscle twitching
- sweating
- shivering
- diarrhoea
If you experience these symptoms, you should stop taking the medicine and seek immediate advice from your GP or specialist. If this is not possible, call NHS 111.
Symptoms of severe serotonin syndrome include:
- seizures (fits)
- irregular heartbeat (arrhythmia)
- unconsciousness
If you experience symptoms of severe serotonin syndrome, seek emergency medical help immediately by dialling 999 to ask for an ambulance.
Hyponatraemia
Elderly people who take antidepressants, particularly those who take SSRIs, may experience a severe fall in sodium (salt) levels, known as hyponatraemia. This may lead to a build-up of fluid inside the cells of the body, which can be potentially dangerous.
This can happen because SSRIs can block the effects of a hormone that regulates levels of sodium and fluid in the body. Elderly people are vulnerable because fluid levels become more difficult for the body to regulate as people age.
Mild hyponatraemia can cause symptoms similar to depression or side effects of antidepressants, such as:
- feeling sick
- headache
- muscle pain
- reduced appetite
- confusion
More severe hyponatraemia can cause:
- feeling listless and tired
- disorientation
- agitation
- psychosis
- seizures (fits)
The most serious cases of hyponatraemia can cause you to stop breathing or enter a coma.
If you suspect mild hyponatraemia, you should call your GP for advice and stop taking SSRIs for the time being.
If you suspect severe hyponatraemia, call 999 and ask for an ambulance.
Hyponatraemia can be treated by feeding a sodium solution into the body through an intravenous drip.
Diabetes
Long-term use of SSRIs and TCAs has been linked to an increased risk of developing type 2 diabetes, although it’s not clear if the use of these antidepressants directly causes diabetes to develop.
It may be that the weight gain some people using antidepressants experience increases the risk of them developing type 2 diabetes.
For more information, see “Claim that antidepressants cause diabetes unproven”.
Suicidal thoughts
In rare cases, some people experience suicidal thoughts and a desire to self-harm when they first take antidepressants. Young people under 25 seem particularly at risk.
Contact your GP, or go to hospital immediately, if you have thoughts of killing or harming yourself at any time while taking antidepressants.
It may be useful to tell a relative or close friend if you’ve started taking antidepressants and ask them to read the leaflet that comes with your medicines. You should then ask them to tell you if they think your symptoms are getting worse, or if they’re worried about changes in your behaviour.
Pain Medications, Pain Relief, and Pain Management