Headaches are associated with more than 300 known medical conditions. Sometimes they are caused by the disease, and sometimes the conditions. One of these conditions is sinusitis, which is commonly misdiagnosed. This is often confused with migraines. Sinus headache symptoms are often caused by full or inflamed sinuses.
Your sinuses are air-filled spaces inside your forehead, cheekbones, and behind the bridge of your nose. When they get inflamed — usually because of an allergic reaction or an infection — they swell, make more mucus, and the channels that drain them can get blocked.
The build-up of pressure in your sinuses causes pain that feels like a headache.
A sinus headache can sometimes be an indicator of a more serious underlying condition. One such condition is a deviated septum, which is a genetic disorder leading to excessive fluid retention in the sinus cavities, essentially a form of sinusitis. If diagnosed with this condition, surgical correction may be an option. For milder cases, managing the symptoms of sinus headaches can often suffice. Applying a warm or cold compress to the affected area can help alleviate swelling and pain. Certain nasal sprays have also demonstrated effectiveness in symptom relief, but it’s crucial not to exceed the recommended dosage, as overuse can potentially worsen the condition.
Environmental factors can contribute to sinus headache symptoms as well. Pressure changes during air travel are a common trigger. Allergens and stress can negatively impact the sinuses, and even weather conditions like humidity and air pressure fluctuations can lead to sinus cavity inflammation, resulting in headaches.
When congested sinuses are the root cause, symptoms typically subside as the sinuses begin to drain. Steam inhalation can sometimes initiate this drainage process. In cases where it doesn’t, antibiotics may be required to reduce excess fluid in the sinuses. If you experience recurring sinus headaches, it’s advisable to consult with your doctor to explore the most suitable treatment options for managing these symptoms.
What is Sinus Headache ?
Sinusitis means your sinuses are inflamed. The cause can be an infection or another problem. Your sinuses are hollow air spaces within the bones surrounding the nose. They produce mucus, which drains into the nose. If your nose is swollen, this can block the sinuses and cause pain.
There are several types of sinusitis, including
- Acute, which lasts up to 4 weeks
- Subacute, which lasts 4 to 12 weeks
- Chronic, which lasts more than 12 weeks and can continue for months or even years
- Recurrent, with several attacks within a year
Acute sinusitis often starts as a cold, which then turns into a bacterial infection. Allergies, nasal problems, and certain diseases can also cause acute and chronic sinusitis.
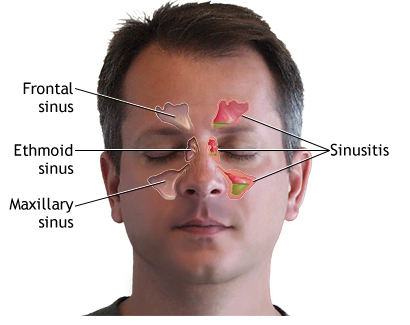
The sinuses are located in several different places. These include behind the eyes and above the nose. The mucus and tissue in these cavities can be filled or irritated, causing much pain. Sometimes the cavities become so full that create the pressure, in turn, causes pain.
These headaches are called secondary headaches when caused by something like a common cold or some other existing medical condition. When the headache is the condition, known as primary headaches. These are also often caused by something else. Be careful not to select one that will actually worsen the effects. Paracetamol and aspirin are effective treatment options, but may be exceeded. MOH (medication overuse headache) is something that affects people that overuse of medications, either in-the-counter or prescription.
Your sinuses are air-filled spaces inside your forehead, cheekbones, and behind the bridge of your nose. When they get inflamed — usually because of an allergic reaction or an infection — they swell, make more mucus, and the channels that drain them can get blocked.
The build-up of pressure in your sinuses causes pain that feels like a headache.
Symptoms of Sinusitis Headache
You’ll feel a deep and constant pain in your cheekbones, forehead, or the bridge of your nose. The pain usually gets stronger when you move your head suddenly or strain. At the same time, you might have other sinus symptoms, such as:
- A runny nose
- Feeling of fullness in your ears
- Fever
- Swelling in your face
Other kinds of recurring headaches, like migraines or tension headaches, are often mistaken for sinus headaches. Because the treatment you need depends on what kind of headache you have, it’s important to figure out if your symptoms are caused by your sinuses. If a sinus blockage, such as an infection, really is the cause, you’ll likely have a fever.
Sinus Headache or Migraine ?
Distinguishing between a sinus headache and a migraine can sometimes be challenging because they can share similar symptoms. However, there are certain characteristics and factors that can help you differentiate between the two:
Sinus Headache:
- Location of Pain: Sinus headaches typically cause pain in the forehead, cheeks, and the area around the eyes and nose. The discomfort may be felt on both sides of the face.
- Quality of Pain: Sinus headaches often produce a constant, dull, aching pain. It may worsen with head movements or when bending forward.
- Accompanying Symptoms: Sinus headaches are usually accompanied by other symptoms of sinusitis, such as nasal congestion, thick yellow or green nasal discharge, facial tenderness or pressure, and a reduced sense of smell and taste.
- Triggers: Sinus headaches are often triggered or worsened by factors like changes in atmospheric pressure (e.g., during weather changes or flights), allergies, infections, or exposure to irritants.
- Duration: Sinus headaches tend to be shorter in duration than migraines and typically improve as the underlying sinus issue resolves.
Migraine:
- Location of Pain: Migraine headaches are commonly described as throbbing or pulsating pain, often on one side of the head, although they can affect both sides. The pain may be concentrated in the temple, behind the eye, or at the base of the skull.
- Quality of Pain: Migraines typically cause moderate to severe pain and are often accompanied by nausea, vomiting, sensitivity to light (photophobia), and sensitivity to sound (phonophobia).
- Aura: Some individuals with migraines experience an aura before or during the headache, which can involve visual disturbances, such as flashing lights or zigzag lines, or sensory changes, like tingling in the face or hands. Not all migraine sufferers experience an aura.
- Triggers: Migraines can be triggered by a wide range of factors, including stress, hormonal changes, certain foods or beverages, lack of sleep, and environmental factors.
- Duration: Migraines can last for several hours to days and are often debilitating.
Causes of Sinus Headache
A sinusitis headache, also known as a sinus headache, is primarily caused by inflammation or infection of the sinuses, which are air-filled cavities located within the facial bones around the nose and eyes. When the sinuses become blocked, inflamed, or infected, they can produce pain and pressure in the forehead, cheeks, and the area around the eyes and nose, leading to a sinus headache. Here are the common causes of sinusitis headaches:
- Sinus Infection (Sinusitis): The most common cause of sinus headaches is sinusitis, which is an inflammation or infection of the sinuses. Sinusitis can occur due to viral, bacterial, or fungal infections. Infections cause the sinuses to become congested and produce excess mucus, leading to pain and pressure.
- Allergies: Allergic reactions to airborne allergens, such as pollen, dust mites, pet dander, and mold, can trigger sinusitis and subsequent sinus headaches. Allergies can cause inflammation and swelling of the sinus passages. You may be sensitive to certain substances. This causes the release of histamine in the body. Histamine makes your sinus and nasal linings swell. Long-term swelling clogs your sinuses. It prevents the tiny hairs (cilia) in the nasal lining from sweeping away mucus. Allergy symptoms can continue over time. But they’re less severe than with colds.
- Nasal Polyps: Nasal polyps are noncancerous growths that can develop in the nasal passages and sinuses. They can obstruct the normal flow of mucus and air through the sinuses, leading to sinusitis and associated headaches.
- Blocked Nasal Passages: Anything that obstructs the normal flow of air and mucus through the nasal passages can contribute to sinusitis and headaches. This can include structural issues like a deviated septum or the presence of foreign bodies.
- Environmental Irritants: Exposure to environmental irritants, such as tobacco smoke, strong odors, or pollution, can irritate the nasal passages and sinuses, leading to inflammation and headaches.
- Changes in Air Pressure: Rapid changes in atmospheric pressure, such as those experienced during air travel or scuba diving, can affect the sinuses and potentially trigger sinus headaches.
- Weather Changes: Some individuals are sensitive to weather changes, particularly shifts in humidity and air pressure, which can cause inflammation in the sinuses and result in headaches.
- Respiratory Infections: Respiratory infections like the common cold or flu can lead to sinusitis and sinus headaches. These infections can cause inflammation in the nasal passages and sinuses.
- Dental Issues: In rare cases, dental problems, such as an infected tooth or a dental abscess, can radiate pain to the sinus area, mimicking a sinus headache.
- Colds and Other Infections : A cold or flu may cause your sinus and nasal linings to swell. Sinus openings can become blocked. This causes mucus to back up. This backed-up mucus becomes an ideal place for bacteria to grow. Thick, yellow, or discolored mucus is one sign of infection.
People with chronic nasal problems or allergies are more likely to get acute sinusitis. Sinusitis is also more common if you have a weakened immune system, such as with HIV. You are also more likely to get sinusitis if you have cystic fibrosis or another condition that causes your body to make extra mucus.
How to Treat Sinusitis Headache ?
Treating a sinusitis headache involves addressing the underlying cause of sinusitis (inflammation or infection of the sinuses) and managing the associated pain and discomfort. Here are steps and strategies to help alleviate sinusitis headaches:
- Consult a Healthcare Provider: If you suspect you have sinusitis or are experiencing severe or persistent symptoms, it’s important to consult a healthcare provider for an accurate diagnosis and appropriate treatment recommendations.
- Address the Underlying Sinusitis:
- Antibiotics: If your sinusitis is bacterial in nature, your doctor may prescribe antibiotics to treat the infection. It’s crucial to complete the full course of antibiotics as prescribed.
- Decongestants: Over-the-counter (OTC) decongestants, like pseudoephedrine, can help reduce nasal congestion and promote sinus drainage. However, they should be used for short durations and according to package instructions to avoid rebound congestion.
- Nasal Steroids: Intranasal corticosteroid sprays, available by prescription or OTC, can help reduce inflammation in the nasal passages and sinuses, relieving congestion and pressure.
- Pain Relief: Over-the-counter pain relievers can help manage the headache pain associated with sinusitis. Options include:
- Acetaminophen: Effective for pain and reducing fever.
- Ibuprofen or Naproxen: Nonsteroidal anti-inflammatory drugs (NSAIDs) that can help reduce pain and inflammation.
- Nasal Irrigation: Saline nasal sprays or nasal irrigation with a neti pot or squeeze bottle can help flush out mucus and debris from the nasal passages, promoting drainage and relieving congestion.
- Humidification: Using a humidifier in your room can add moisture to the air, which may help alleviate dryness and congestion in the nasal passages.
- Warm Compresses: Applying a warm, moist compress to your forehead, cheeks, and sinus areas can help reduce pain and pressure. Use a warm washcloth or a microwaveable heating pad.
- Hydration: Staying well-hydrated can help keep mucus thin and easier to expel. Drink plenty of fluids, such as water, herbal teas, and clear broths.
- Rest: Give your body adequate rest to recover from sinusitis. Rest can help boost your immune system’s ability to fight off the infection.
- Avoid Irritants: Steer clear of environmental irritants like tobacco smoke and strong odors, as these can exacerbate sinusitis symptoms.
- Allergy Management: If allergies contribute to your sinusitis, identify and manage allergens that trigger your symptoms. This may include allergen avoidance, using allergy medications, or exploring allergy immunotherapy (allergy shots).
- Elevate Your Head: Sleeping with your head elevated can help reduce nasal congestion and promote sinus drainage.
- Consider Saline Nasal Sprays: OTC saline nasal sprays or saline gels can provide relief by moisturizing and soothing irritated nasal passages.
If your symptoms persist or worsen despite these self-care measures, or if you develop severe symptoms such as high fever, severe facial pain, or visual disturbances, it’s essential to seek medical attention promptly. These may be signs of a more severe sinus infection or a complication that requires medical intervention.
How to Prevent Sinusitis Headache ?
Preventing sinusitis headaches involves taking measures to reduce the risk of developing sinusitis, which is the underlying cause of these headaches. Here are some strategies to help prevent sinusitis and, consequently, sinusitis headaches:
- Maintain Good Nasal Hygiene:
- Nasal Irrigation: Regularly use saline nasal sprays or perform nasal irrigation with a neti pot or squeeze bottle to keep the nasal passages clear of mucus and irritants. This can help prevent congestion and promote proper sinus drainage.
- Stay Hydrated:
- Drink an adequate amount of water and stay well-hydrated. Proper hydration helps keep the mucus in your nasal passages thin and easy to expel.
- Manage Allergies:
- Identify and manage allergens that trigger your allergic rhinitis (allergic inflammation of the nasal passages), as allergic reactions can lead to sinusitis. This may involve allergen avoidance, using allergy medications, or exploring allergy immunotherapy (allergy shots).
- Reduce Irritants:
- Avoid or minimize exposure to environmental irritants, such as tobacco smoke, strong odors, and pollution, as these can irritate the nasal passages and increase the risk of sinusitis.
- Hand Hygiene:
- Practice good hand hygiene by washing your hands frequently, especially during cold and flu seasons, to reduce the risk of infection that can lead to sinusitis.
- Humidify Your Environment:
- Use a humidifier in your living space, particularly during the dry winter months. Adding moisture to the air can help prevent dry nasal passages and congestion.
- Avoid Overuse of Decongestant Nasal Sprays:
- Overuse of over-the-counter decongestant nasal sprays can lead to a condition called “rebound congestion.” This makes nasal congestion worse when you stop using the spray. Limit the use of these sprays to a few days, and consult a healthcare provider if congestion persists.
- Manage Respiratory Infections:
- Practice good respiratory hygiene, such as covering your mouth and nose when coughing or sneezing, and disposing of tissues properly. This helps prevent the spread of infections that can lead to sinusitis.
- Consider Allergy-Proofing Your Home:
- Take steps to reduce allergens in your home, such as using allergen-proof pillow and mattress covers, regularly cleaning and dusting, and ensuring good ventilation.
- Stay Informed:
- Be aware of weather changes and factors like high pollen counts, which can trigger sinusitis in some individuals. Take precautions or adjust your activities accordingly during times when sinusitis triggers are more prevalent.
- Manage Stress:
- Chronic stress can weaken the immune system, making you more susceptible to infections. Engage in stress-reduction techniques like meditation, yoga, or deep breathing exercises.
- Stay Up to Date on Immunizations:
- Keeping up with recommended vaccinations, including flu and pneumonia vaccines, can help prevent respiratory infections that may lead to sinusitis.
If you have a history of recurrent sinusitis or sinusitis headaches, it’s advisable to consult with an ear, nose, and throat specialist (otolaryngologist) or an allergist for further evaluation and personalized recommendations for prevention. They can assess your specific risk factors and provide guidance tailored to your needs.
Risk Factors of Sinus Headache ?
Several risk factors can increase the likelihood of experiencing sinus headaches, which are typically associated with sinusitis (inflammation or infection of the sinuses). Understanding these risk factors can help individuals take preventive measures and manage their sinus health more effectively. Common risk factors for sinus headaches include:
- Sinusitis: The most significant risk factor for sinus headaches is sinusitis itself. Chronic or recurrent sinusitis, whether it’s due to viral, bacterial, or fungal infections or other causes, can lead to frequent bouts of sinus headaches.
- Allergies: Allergic rhinitis (hay fever) is a risk factor for sinusitis and sinus headaches. Allergic reactions to airborne allergens, such as pollen, dust mites, pet dander, and mold, can trigger sinus inflammation.
- Environmental Irritants: Exposure to irritants like tobacco smoke, strong odors, pollution, and chemical fumes can irritate the nasal passages and sinuses, increasing the risk of inflammation and sinusitis.
- Nasal Obstruction: Structural issues in the nasal passages, such as a deviated septum, nasal polyps, or foreign bodies, can obstruct airflow and mucus drainage, making the sinuses more susceptible to infection and inflammation.
- Respiratory Infections: Frequent upper respiratory infections, such as the common cold or flu, can lead to sinusitis and sinus headaches. These infections can cause inflammation in the nasal passages and sinuses.
- Weather Changes: Some individuals are sensitive to weather changes, particularly shifts in humidity and air pressure. These changes can affect the sinuses and contribute to sinus headaches.
- Low Immune Function: A weakened immune system, whether due to a medical condition or medications that suppress the immune response, can increase the risk of sinus infections and associated headaches.
- Age: Children and older adults may be at a higher risk of developing sinus infections and related headaches. In children, immature immune systems and exposure to respiratory infections can contribute to sinusitis. In older adults, age-related changes in sinus structure and function may increase vulnerability.
- Family History: A family history of sinusitis or a tendency toward allergies can be a genetic risk factor for sinus headaches.
- Occupational Exposure: Certain occupations that involve exposure to dust, allergens, or environmental irritants may pose a higher risk of sinusitis and sinus headaches. This includes jobs in construction, agriculture, and manufacturing.
- Immune Disorders: Individuals with underlying immune disorders, such as HIV/AIDS or autoimmune diseases, may be more susceptible to sinusitis and sinus headaches due to impaired immune function.
- Cystic Fibrosis: Cystic fibrosis is a genetic disorder that can lead to thick, sticky mucus production in the respiratory system, including the sinuses, making individuals more prone to sinusitis.
It’s important to note that while these risk factors can increase the likelihood of sinus headaches, not everyone with these risk factors will necessarily develop sinusitis or experience sinus headaches.