What is Migraine?
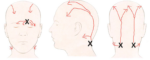
Migraine is a type of headache characterized by recurrent attacks of moderate to severe throbbing and pulsating pain on one side of the head. The pain is caused by the activation of nerve fibers within the wall of brain blood vessels traveling inside the meninges (three layers of membranes protecting the brain and spinal cord).
Untreated attacks last from four to 72 hours. Other common symptoms include:
- Increased sensitivity to light, noise, and odors
- Nausea
- Vomiting
Routine physical activity, movement, or even coughing or sneezing can worsen the headache pain.
Migraines occur most frequently in the morning, especially upon waking. Some people have migraines at predictable times, such as before menstruation or on weekends following a stressful week of work. Many people feel exhausted or weak following a migraine but are usually symptom-free between attacks.
A number of different factors can increase your risk of having a migraine. These factors, which trigger the headache process, vary from person to person and include:
Migraine is divided into four phases, all of which may be present during the attack:
- Premonitory symptoms occur up to 24 hours prior to developing a migraine. These include food cravings, unexplained mood changes (depression or euphoria), uncontrollable yawning, fluid retention, or increased urination.
- Aura—Some people will see flashing or bright lights or what looks like heat waves immediately prior to or during the migraine, while others may experience muscle weakness or the sensation of being touched or grabbed.
- Headache—A migraine usually starts gradually and builds in intensity. It is possible to have migraine without a headache.
- Postdrome—Individuals are often exhausted or confused following a migraine. The postdrome period may last up to a day before people feel healthy again.

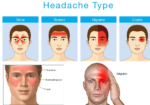
The Types of Migraines
The two major types of migraine are:
- Migraine with aura, previously called classic migraine, includes visual disturbances and other neurological symptoms that appear about 10 to 60 minutes before the actual headache and usually last no more than an hour. Individuals may temporarily lose part or all of their vision. The aura may occur without headache pain, which can strike at any time. Other classic symptoms include trouble speaking; an abnormal sensation, numbness, or muscle weakness on one side of the body; a tingling sensation in the hands or face, and confusion. Nausea, loss of appetite, and increased sensitivity to light, sound, or noise may precede the headache.
- Migraine without aura, or common migraine, is the more frequent form of migraine. Symptoms include headache pain that occurs without warning and is usually felt on one side of the head, along with nausea, confusion, blurred vision, mood changes, fatigue, and increased sensitivity to light, sound, or noise.
Other types of migraine include:
- Abdominal migraine mostly affects young children and involves moderate to severe pain in the middle of the abdomen lasting one to 72 hours, with little or no headache. Additional symptoms include nausea, vomiting, and loss of appetite. Many children who develop abdominal migraine will have migraine headaches later in life.
- Basilar-type migraine mainly affects children and adolescents. It occurs most often in teenage girls and may be associated with their menstrual cycle. Symptoms include partial or total loss of vision or double vision, dizziness and loss of balance, poor muscle coordination, slurred speech, a ringing in the ears, and fainting. The throbbing pain may come on suddenly and is felt on both sides at the back of the head.
- Hemiplegic migraine is a rare and severe form of migraine that causes temporary paralysis—sometimes lasting several days—on one side of the body prior to or during a headache. Symptoms such as vertigo, a pricking or stabbing sensation, and problems seeing, speaking, or swallowing may begin prior to the headache pain and usually stop shortly thereafter. When it runs in families the disorder is called familial hemiplegic migraine (FHM). Though rare, at least three distinct genetic forms of FHM have been identified. These genetic mutations make the brain more sensitive or excitable, most likely by increasing brain levels of a chemical called glutamate.
- Menstrual migraine affects women around the time of their period, although most women with menstrually-related migraine also have migraines at other times of the month. Symptoms may include migraine without aura, pulsing pain on one side of the head, nausea, vomiting, and increased sensitivity to sound and light.
- Migraine without headache is characterized by visual problems or other aura symptoms, nausea, vomiting, and constipation, but without head pain.
- Ophthalmoplegic migraine an uncommon form of migraine with head pain, along with a droopy eyelid, large pupil, and double vision that may last for weeks, long after the pain is gone.
- Retinal migraine is a condition characterized by attacks of visual loss or disturbances in one eye. These attacks, like the more common visual auras, are usually associated with migraine headaches.
- Status migrainosus is a rare and severe type of acute migraine in which disabling pain and nausea can last 72 hours or longer. The pain and nausea may be so intense that people need to be hospitalized.
Who is at a Higher Risk of Experiencing Migraines?
Migraines can affect both children and adults, but they are more prevalent among adult women, occurring three times more frequently than in men. Migraines often have a genetic component, with many individuals having a family history of the condition. They also tend to co-occur with other medical conditions, including depression, anxiety, bipolar disorder, sleep disorders, and epilepsy, at higher rates than in the general population. People who experience pre-migraine symptoms known as aura may have a slightly elevated risk of suffering a stroke.
In women, migraines are often associated with hormonal changes. These headaches can commence with the onset of the first menstrual cycle or during pregnancy. Most women experience improvements in migraine symptoms after menopause, but surgical removal of the ovaries can exacerbate them. Additionally, women who have migraines and use oral contraceptives may notice changes in the frequency and severity of their attacks, while some women who do not have a history of headaches may develop migraines as a side effect of oral contraceptive use.
How is Migraine Treated?
The treatment of migraines focuses on alleviating symptoms and preventing future attacks. Here are some steps to quickly ease migraine symptoms:
- Rest in a Quiet, Dark Room: Napping or resting with your eyes closed in a quiet, darkened room can help reduce discomfort.
- Apply a Cold Compress: Placing a cool cloth or ice pack on your forehead can provide relief.
- Stay Hydrated: Drink plenty of fluids, especially if you experience vomiting during the migraine.
- Consider Caffeine: Small amounts of caffeine may help alleviate symptoms, particularly during the early stages of a migraine.
Migraine medication strategies encompass acute and preventive approaches. Acute medications, also known as “abortive” treatments, are taken at the onset of symptoms to alleviate pain and restore normal functioning. Preventive treatment involves daily medication to reduce the intensity and frequency of future migraine episodes. The U.S. Food and Drug Administration (FDA) has sanctioned several drugs for migraine management, including enenmab (Aimovig) and galcanezumab-gnlm (Emgality) for preventive use, as well as lasmiditan (Reyvow) and ubrogepant (Ubrelvy) tablets for short-term relief from migraines, with or without aura. To ensure safe usage, it is advisable for individuals using migraine medications to be under the supervision of a healthcare professional due to potential side effects associated with these drugs.
The Acute Treatment of Migraine
The acute treatment options for migraines encompass various medications to address different aspects of migraine pain and discomfort:
- Triptan Drugs: Triptans are favored for migraine relief as they boost serotonin levels in the brain, leading to blood vessel constriction and a reduced pain threshold. They effectively alleviate moderate to severe migraine pain.
- Ergot Derivative Drugs: These medications bind to serotonin receptors on nerve cells, thereby reducing the transmission of pain signals along nerve fibers. Ergot derivatives are particularly effective when administered during the early stages of a migraine.
- Over-the-Counter Analgesics: Non-prescription pain relievers like ibuprofen, aspirin, or acetaminophen can provide relief for milder migraine headaches.
- Combination Analgesics: This category includes a blend of medications, such as acetaminophen combined with caffeine and/or a narcotic. These combination analgesics are suitable for migraines that do not respond well to simple analgesics.
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): NSAIDs are known for their ability to reduce inflammation and alleviate pain, making them useful for migraine management.
- Nausea Relief Medications: Certain drugs are designed to combat queasiness associated with various headache types, offering relief from accompanying symptoms.
- Narcotics: Narcotic medications may be prescribed briefly to relieve severe pain during a migraine episode. However, they are not recommended for the treatment of chronic headaches due to the risk of dependence and other side effects.
It’s essential to note that while these medications can be effective for acute migraine relief, their usage should align with medical advice and recommendations. Chronic headache management typically involves a different approach and may include preventive measures in addition to acute treatments. Consulting with a healthcare provider for a personalized migraine management plan is crucial for individuals suffering from migraines.
All individuals experiencing migraines require prompt and effective treatment during headache episodes. For those with frequent and severe migraines, preventive medications may be necessary. In general, preventive measures should be considered if migraines occur at least once a week or are less frequent but highly debilitating. Additionally, individuals who find themselves using headache treatments more than three times a week are advised to explore preventive medications. Physicians typically recommend trying one or more preventive medications for a duration of two to three months to evaluate their effectiveness, unless intolerable side effects are encountered.
The Preventive Treatment of Migraines
Several preventive medications initially intended for other conditions have shown efficacy in managing migraines:
- Anticonvulsants: Originally developed to treat epilepsy, anticonvulsant drugs have been found to be beneficial for individuals with various headache types, including migraines. These medications work by increasing the levels of specific neurotransmitters and reducing pain signals.
- Beta-blockers: Typically prescribed for high blood pressure, beta-blockers have demonstrated effectiveness in migraine prevention.
- Calcium channel blockers: These drugs are used to manage high blood pressure and contribute to stabilizing the walls of blood vessels. Their mechanism of action involves preventing blood vessels from excessive narrowing or widening, which can impact blood flow to the brain.
- Antidepressants: While antidepressants primarily target brain chemicals related to mood regulation, their role in migraine treatment is not directly associated with their impact on mood. Antidepressants may benefit individuals with other headache types because they enhance serotonin production and influence the levels of other chemicals like norepinephrine and dopamine.
These medications, when prescribed by a healthcare professional, can be valuable tools in preventing and managing migraines and related headache disorders.
The Natural Treatments for Migraine
Natural treatments for migraines can be used in conjunction with medical therapies or as standalone approaches for prevention and relief. Here are some natural remedies that may help manage migraines:
- Dietary Modifications: Certain foods and drinks can trigger migraines in some individuals. Keeping a food diary to identify triggers and avoiding them can be helpful. Common triggers include aged cheeses, processed meats, alcohol, and caffeine.
- Hydration: Dehydration can trigger migraines in some people. Staying well-hydrated by drinking plenty of water throughout the day is important.
- Regular Meals: Skipping meals can lead to low blood sugar, which may trigger migraines. Eating regular, balanced meals can help stabilize blood sugar levels.
- Caffeine Management: While some people find that caffeine helps relieve migraines, excessive caffeine intake or caffeine withdrawal can also trigger headaches. Moderation is key.
- Adequate Sleep: Poor sleep patterns, including both too much and too little sleep, can be migraine triggers. Establishing a consistent sleep schedule and improving sleep hygiene can be beneficial.
- Stress Reduction: Stress is a common migraine trigger. Stress management techniques such as yoga, meditation, deep breathing exercises, and progressive muscle relaxation may help.
- Physical Activity: Regular exercise can reduce the frequency and severity of migraines. However, intense exercise can also trigger migraines in some individuals, so it’s important to find a balance that works for you.
- Herbal Remedies: Some herbs, such as butterbur and feverfew, have been studied for their potential migraine-preventing effects. Always consult with a healthcare provider before trying herbal supplements.
- Acupuncture: Acupuncture is a traditional Chinese medicine practice that involves inserting thin needles into specific points on the body. Some people find it helpful in reducing migraine frequency and severity.
- Biofeedback: Biofeedback is a technique that helps individuals learn how to control physiological functions, such as muscle tension and heart rate, to reduce migraine frequency and intensity.
- Essential Oils: Certain essential oils, such as lavender and peppermint, are believed to have headache-relieving properties. Diluted oils can be applied topically or inhaled.
- Magnesium Supplements: Some migraine sufferers have low magnesium levels. Consult a healthcare provider before taking magnesium supplements, as excessive magnesium intake can have side effects.
- Riboflavin (vitamin B2) – Some individuals with migraines may have lower levels of riboflavin in their bodies, and supplementation may help reduce the frequency and severity of migraine attacks.
- Coenzyme Q10 – It has been studied as a potential supplement for migraine prevention, and some individuals with migraines have reported benefits from CoQ10 supplementation.
- Butterbur (medicinal plant) – is a perennial herb that has been used historically for various medicinal purposes, including migraine prevention. It has gained attention as a potential natural treatment for migraines, and some studies suggest that it may be effective in reducing the frequency and severity of migraine attacks.
It’s essential to remember that what works for one person may not work for another. Migraine management is highly individualized, and consulting with a healthcare professional is crucial, especially if migraines are severe, frequent, or significantly affecting your quality of life. They can help create a tailored treatment plan that may include a combination of natural and medical interventions.
Pain Medications, Pain Relief, and Pain Management