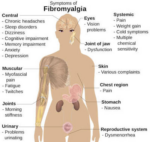
Fibromyalgia syndrome (FMS) is originally a disorder of sensory amplification in which heightened sensory input leads to a complex array of symptoms, including pain, fatigue, insomnia, and mood disorders. (1) This broad range of clinical manifestations can make fibromyalgia syndrome difficult to cure and usually needs a multi disciplinary approach to remedy. A rational therapeutic plan will aim at both the underlying sensory amplification disorder and the resultant functional symptoms.
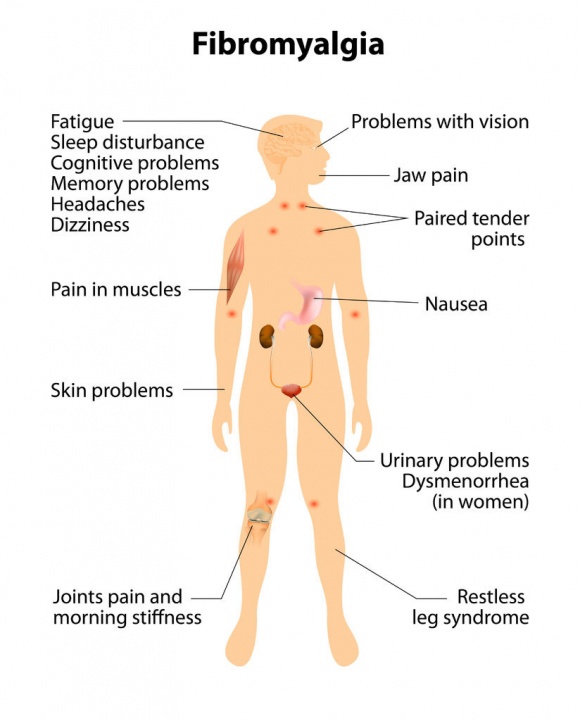
The study of pain pathways is an area of great interest for fibromyalgia researchers, and along with genetics, provides significant hope for advancement in the diagnosis and treatment of FMS. Current research indicates that dysfunctional sensory amplification can occur via several neurochemical pathways, and treatment modalities usually involve pharmacologic manipulation of these neurochemicals.
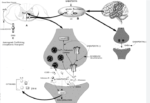
Recently, much of the focus has been centered on the serotonin-norepinephrine descending pain pathway. (2) In this pain processing pathway, serotonin and norepinephrine are used by the brain as intermediaries to inhibit pain signals from the body. Deficiencies of serotonin or norepinephrine cause this feedback mechanism to misfire, and pain processing signals remain unregulated.
This has sparked interest among clinicians because some studies indicate that serum levels of serotonin and norepinephrine are diminished in fibromyalgia patients. Subsequent clinical trials with medications that modulate serotonin and norepinephrine (i.e. amitriptyline, duloxetine, venlafaxine) have proven beneficial to some subjects. (3,4)
Another area of active research involves the voltage-dependent calcium channel which controls the release of excitatory neurotransmitters involved in pain processing, including glutamate and substance P. Inhibiting the release of these compounds decreases pain signal processing. Pregabalin and gabapentin are the two primary medications of this class used in fibromyalgia patients.
One of the more troubling aspects of developing effective treatments is the idea that fibromyalgia syndrome can affect more than one pain processing pathway, and further, the pathways involved may not be the same for each patient. So, a medication that works reasonably well in one patient may be completely ineffective (or detrimental) in another.
Genetic research into fibromyalgia even raises the possibility of multiple etiologies for FMS. Several different genetic markers are under study, and it is possible that not a single gene, but a variable combination of genes, is responsible for the expression of fibromyalgia syndrome. (5,6,7,8) Simply stated, the root cause of fibromyalgia may not be the same for all patients.
Because the currently available treatments for primary pain provide incomplete relief, attention also must be given to treating the functional symptoms of fibromyalgia syndrome. The treatment of pain amplification disorder is almost exclusively the domain of pharmacology, but the broad nature of related functional symptoms invites the use of many treatment modalities, both pharmacologic and non-pharmacologic.
It is easy to imagine how a pain amplification disorder like fibromyalgia syndrome could cause otherwise sub-clinical ailments to become symptomatic and require treatment. For instance, a headache in a hyper sensitized fibromyalgia patient might be experienced as intolerably painful, while the same headache in a person with normal pain processing pathways might be perceived as only a nuisance.
Of course, this is an oversimplification. The connection between fibromyalgia and other conditions (like depression) involves both genetics and endocrinology, and is not just a result of heightened pain sensations, but the point is that fibromyalgia syndrome has the potential to adversely effect virtually any system in the body.
Treatment of these functional symptoms is primarily symptomatic or palliative in nature, and since not everyone has the same symptoms, the treatment must be individualized. This variability accounts, at least in part, for the numerous testimonials and miracle cures found online. It may be possible to virtually eliminate a particular functional symptom of fibromyalgia without correcting the underlying pathology. Confusion arises when this is mistaken as a “cure” for fibromyalgia syndrome.
Some of the more popular treatment modalities for these functional symptoms include:
- Pharmacologic agents
- Education
- Cognitive Behavioral Therapy
- Nutrition & Dietary Supplements
- Biofeedback
- Exercise Programs
- Therapeutic Yoga
- Massage Therapy
- Acupuncture
- Electro therapy
It is important to remember that the treatment must be individualized when addressing these symptoms. Therapies will not always have the same effect on individual fibromyalgia patients. The only way to arrive at a truly optimized treatment plan is through trial-and-error. Understanding this before treatment begins should help fibromyalgia patients keep a positive attitude while sorting through the broad collection of available treatments.
Due to the variable etiology and expression of fibromyalgia syndrome, finding effective treatments can be difficult. Dividing treatment goals into two categories- reduction of primary pain amplification, and reduction of resulting functional symptoms- can clarify the procedure, and allow for the individualized development of an optimal therapeutic plan.
1. Lawson K. Treatment options and patient perspectives in the management of fibromyalgia: future trends. Neuropsychiatr Dis Treat. 2008 Dec;4(6):1059-71.
2. Senba E, Imbe H, Okamoto K. Descending facilitation in chronic stress and chronic pain state. Nihon Shinkei Seishin Yakurigaku Zasshi. 2008 Feb;28(1):29-35.
3. Russell IJ, Vaeroy H, Javors M, Nyberg F. Cerebrospinal fluid biogenic amine metabolites in fibromyalgia/fibrositis syndrome and rheumatoid arthritis. Arthritis Rheum. 1992 May;35(5):550-60.
4. Hauser W, Bernardy K, Uceyler N, Sommer C. Treatment of fibromyalgia syndrome with antidepressants: a meta-analysis. JAMA. 2009 Jan 14;301(2):198-209.
5. Bondy et al. The T102c polymorphism of the 5-HT2A-receptor gene in fibromyalgia. Neurobiol. Dis. 1999;6:433-439.
6. Offenbaecher et al. Possible association of fibromyalgia with a polymorphism in the seratonin transporter gene regulatory region. Arthritis Rheum. 1999;42:2482-2488.
7. Buskilla et al. An association between fibromyalgia and the dopamine D4 receptor exon III repeat polymorphism and relationship to novelty seeking behavior. Mol. Psychiatry 2004;9:73.
8. Gursoy et al. Significance of catecholamine o-methyl transferase gene polymorphism in fibromyalgia syndrome. Rheumatol. Int. 2003;23:104-107.
Pain Medications, Pain Relief, and Pain Management